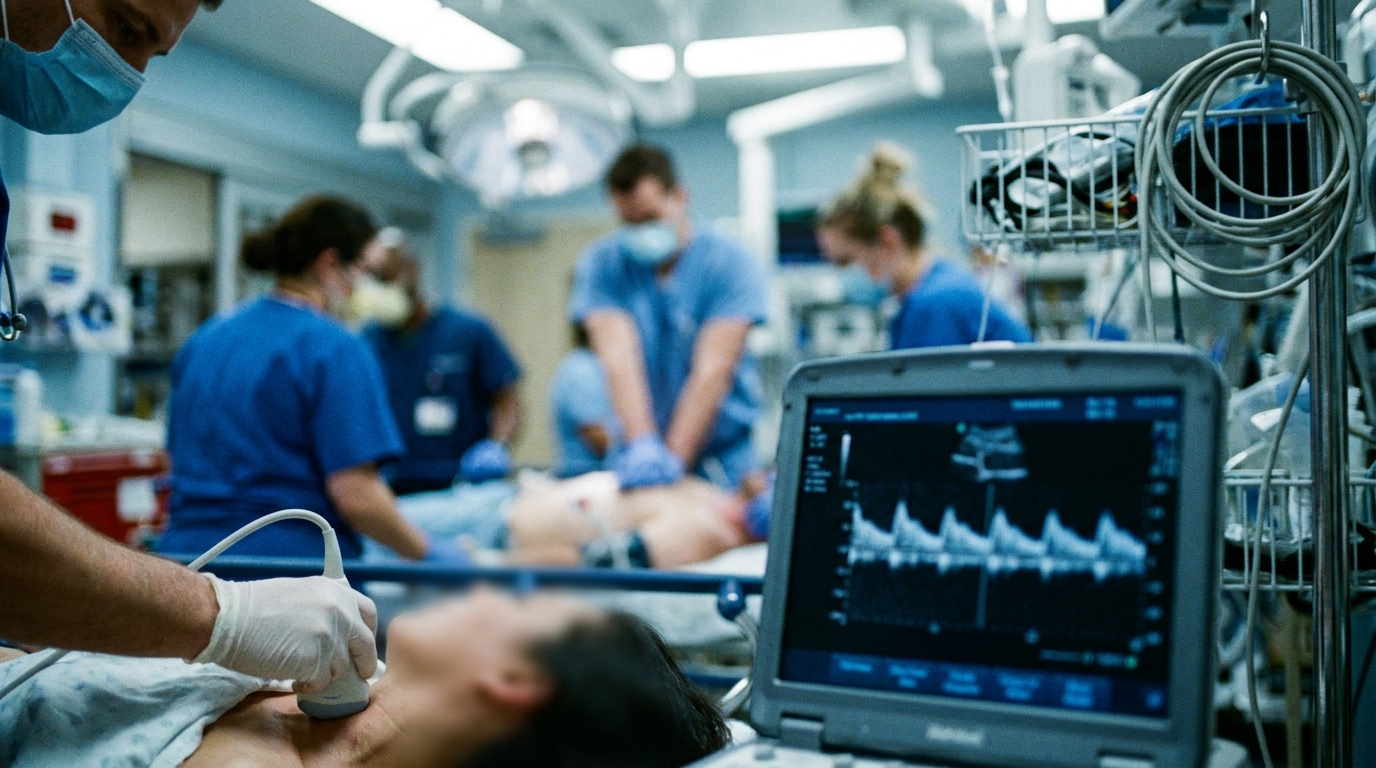
- Clinicians need non-invasive methods to monitor hemodynamic efficacy and predict the return of spontaneous circulation during cardiopulmonary resuscitation.
- This prospective observational study evaluated carotid Doppler ultrasound parameters in 51 adult patients undergoing cardiopulmonary resuscitation in an emergency department.
- The velocity time integral achieved an area under the curve of 0.811 with an optimal cutoff value of 18.8.
- Researchers concluded that carotid blood flow parameters differ significantly (p < 0.05) between patients who achieve circulation return and those who do not.
- These hemodynamic indicators require multicenter validation because measurements may have overlapped with spontaneous flow during the transition to circulation return.
Hemodynamic Monitoring During Cardiac Arrest
Optimizing cardiopulmonary resuscitation requires precise, real-time feedback on perfusion to guide chest compressions and pharmacological interventions [1]. While invasive hemodynamic monitoring is a standard in some critical care settings, its use during active cardiac arrest is often impractical [2, 3]. Clinicians frequently rely on manual palpation of major arteries to assess for the return of spontaneous circulation, a technique subject to inter-operator variability that necessitates frequent, potentially detrimental pauses in compressions [1, 4]. To address this gap, point-of-care ultrasound offers a non-invasive alternative to quantify blood flow more objectively [5, 6]. A recent prospective study involving 51 adult patients evaluated how specific carotid artery Doppler parameters could serve as physiological indicators of resuscitation success, with a particular focus on the velocity time integral, a measure of the distance blood travels with each compression, which demonstrated good predictive value (area under the curve of 0.811) for achieving return of spontaneous circulation [5].
Prospective Evaluation of Resuscitation Waveforms
To investigate the clinical utility of these non-invasive metrics, researchers conducted a prospective observational study in the emergency department of a tertiary hospital in Zhejiang Province. They enrolled adult patients undergoing cardiopulmonary resuscitation between March 2024 and March 2025, aiming to capture data in a high-acuity environment. The cohort of 51 patients was divided based on clinical outcome: 23 patients achieved return of spontaneous circulation (ROSC), defined as the first documented pulse or functional rhythm at a scheduled check, while 28 patients did not. This definition ensured that the ultrasound findings served as predictors rather than as part of the diagnostic criteria for ROSC.
The analysis revealed that several carotid blood flow parameters differed significantly between the two groups. Metrics such as the velocity time integral (VTI), peak systolic velocity (Vmax), end-diastolic velocity (Vmin), time-averaged velocity (TAV), mean diameter (MD*), resistive index (RI), and maximum acceleration (dv.MAX) were all statistically different between the ROSC and non-ROSC cohorts (all p < 0.05). To assess how well these indicators could distinguish between outcomes, the authors used receiver operating characteristic (ROC) curve analysis, a statistical method that measures a test's diagnostic accuracy. The VTI, which reflects the volume of blood moved per compression, showed the strongest predictive capacity with an area under the curve (AUC) of 0.811. An AUC of 1.0 represents a perfect test, while 0.5 is equivalent to chance. Other parameters also demonstrated utility, including Vmax (AUC 0.758) and Vmin (AUC 0.727), providing quantitative data that correlate with the likelihood of successful resuscitation.
Predictive Accuracy of Carotid Flow Metrics
While these findings suggest that Doppler parameters could provide objective targets for resuscitation quality, a key methodological detail requires careful consideration. The study protocol analyzed a prespecified 60-second Doppler window immediately preceding the clinically documented return of spontaneous circulation. Because ROSC was only confirmed during scheduled pauses for pulse and rhythm checks, it is possible that a patient's own spontaneous circulation had already begun during the final minute of compressions. This phenomenon, known as transition flow, means the ultrasound may have captured a mixture of compression-generated flow and the patient's emerging cardiac output, which could potentially inflate the predictive accuracy of the measured parameters.
Despite this limitation, the study highlights that carotid Doppler can offer valuable, objective hemodynamic insights during CPR without the need for invasive arterial lines. The identified cutoff values, such as 18.8 for VTI and 87.1 for Vmax, could one day help clinicians assess the physiological efficacy of their efforts in real time. However, the authors appropriately categorize these findings as exploratory. Given the single-center design and the potential confounding effect of transition flow, the results require prospective, multicenter validation before these specific ultrasound metrics can be integrated into standard resuscitation protocols to guide clinical decision-making during cardiac arrest.
Clinical Considerations and Transition Flow
The methodology of the study involved a prespecified 60-second Doppler window immediately preceding the documented return of spontaneous circulation for analysis. A critical consideration in interpreting these metrics is the timing of clinical assessment. Because the return of spontaneous circulation was adjudicated only at scheduled pulse and rhythm checks, the Doppler window may have partially overlapped with spontaneous flow rather than capturing purely compression-generated flow. This phenomenon, often referred to as transition flow, occurs because the physiological return of a pulse can happen at any point between formal rhythm checks, meaning the ultrasound may have recorded the patient's own emerging cardiac output alongside manual resuscitation efforts.
Despite the potential for overlapping flow states, the researchers concluded that carotid Doppler parameters provide objective hemodynamic insights during CPR, offering a quantifiable method to assess perfusion quality without the need for invasive arterial lines. These metrics allow clinicians to monitor the physiological impact of chest compressions in real time. However, the authors maintain that these findings are considered exploratory and should be interpreted with caution. Given the single-center nature of the study and the specific timing of the data capture, these parameters require prospective multicenter validation before they can be reliably integrated into standard emergency resuscitation protocols or used to guide definitive clinical decisions during cardiac arrest.
References
1. Li Y, Xie M, Wang G, et al. Evaluating hands-free carotid Doppler ultrasound for real-time return of spontaneous circulation detection in in-hospital cardiac arrest: a multicenter randomized controlled study.. Resuscitation. 2026. doi:10.1016/j.resuscitation.2026.111016
2. Zhang Y, Wang Y, Shi J, Hua Z, Xu J. Cardiac output measurements via echocardiography versus thermodilution: A systematic review and meta-analysis. PLoS ONE. 2019. doi:10.1371/journal.pone.0222105
3. Lorusso R, Shekar K, MacLaren G, et al. ELSO Interim Guidelines for Venoarterial Extracorporeal Membrane Oxygenation in Adult Cardiac Patients. ASAIO Journal. 2021. doi:10.1097/mat.0000000000001510
4. (HRS) AHRS, societies EBTF, (EuSEM) ESOEM, et al. Guidelines for the diagnosis and management of syncope (version 2009): The Task Force for the Diagnosis and Management of Syncope of the European Society of Cardiology (ESC). European Heart Journal. 2009. doi:10.1093/eurheartj/ehp298
5. Zhou S, Wang S, Xu S, et al. Predictive value of carotid artery Doppler ultrasound for resuscitation outcomes in patients with cardiac arrest.. Scandinavian journal of trauma, resuscitation and emergency medicine. 2026. doi:10.1186/s13049-026-01620-6
6. Polito A, Ricci Z, Chiara LD, et al. Cerebral blood flow during cardiopulmonary bypass in pediatric cardiac surgery: the role of transcranial Doppler – a systematic review of the literature. Cardiovascular Ultrasound. 2006. doi:10.1186/1476-7120-4-47