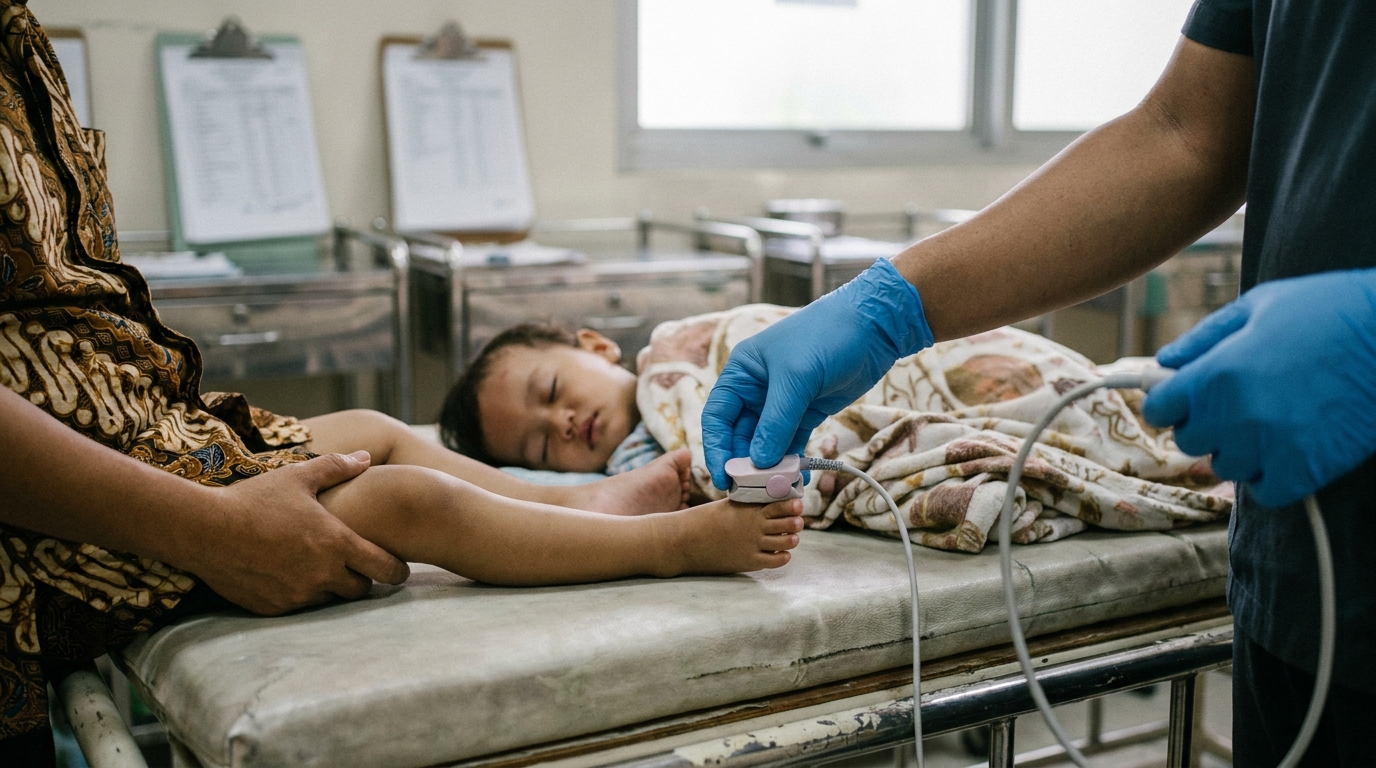
For Doctors in a Hurry
- Current World Health Organization danger signs for febrile children in resource-limited settings often lead to missed severe illness or unnecessary referrals.
- Researchers developed clinical prediction models using data from 3,405 children aged 1 to 59 months across five Asian countries.
- Pulse oximetry models achieved 88.9% sensitivity (95% CI: 76.7-97.8) and a threefold reduction in unnecessary referral rates.
- The researchers concluded that integrating simple clinical parameters or biomarkers improves triage accuracy compared to standard World Health Organization criteria.
- These cost-effective triage tools require further evaluation in community-based trials to confirm their utility in low-resource clinical environments.
Refining Pediatric Triage in Resource-Constrained Febrile Illness
Acute febrile illness remains a primary cause of pediatric morbidity and mortality in low-resource settings, where distinguishing self-limiting infections from life-threatening conditions is a constant clinical challenge [1, 2]. While early identification and management improve outcomes in septic patients, the lack of objective diagnostic tools often leads to either missed severe disease or the inappropriate use of secondary care resources [3, 4]. Current triage strategies frequently rely on broad clinical signs that lack the specificity needed to manage the high volume of patients seen in primary care [5]. Furthermore, underlying factors such as malnutrition can alter immune responses and mask typical clinical presentations, complicating the referral process [6]. To address this gap, researchers have developed and validated a refined clinical prediction model to better identify which febrile children require urgent escalation of care.
Limitations of Current WHO Danger Signs
In resource-constrained community settings, identifying which febrile children require urgent referral to higher-level facilities remains a major unmet need for frontline clinicians. The current triage process largely relies on the World Health Organization (WHO) danger signs, a set of clinical indicators designed to flag children at high risk of mortality. However, researchers found that these established WHO danger signs have limited accuracy, often failing to distinguish between self-limiting conditions and life-threatening infections. In a study of 3,405 children aged 1 to 59 months presenting with community-acquired acute febrile illnesses across Bangladesh, Cambodia, Indonesia, Laos, and Vietnam, the WHO criteria demonstrated a sensitivity of only 55.5% (95% confidence interval (CI): 39.4-72.7) and a specificity of 82.6% (95% CI: 77.1-87.6) for identifying those at risk of rapid deterioration.
The clinical consequences of these diagnostic limitations are twofold: they lead to missed cases of severe illness and generate a high volume of unnecessary referrals that can overwhelm secondary care systems. To evaluate the efficacy of triage tools, the study defined severe disease as death or the requirement for organ support within 2 days of presentation. Because the standard WHO protocols missed nearly half of the children who met this definition of severe disease, there is a critical requirement for more precise clinical prediction models. For practicing physicians, improving the sensitivity of these tools is essential for ensuring that critically ill pediatric patients receive timely intervention, while increasing specificity helps preserve limited hospital resources by reducing the burden of patients who do not require intensive medical management.
Model Development and Multi-Country Validation
To address the diagnostic gaps in existing triage protocols, researchers developed and validated clinical prediction models using a robust dataset from 3,405 children aged 1 to 59 months. This study population consisted of pediatric patients presenting with community-acquired acute febrile illnesses to seven different hospitals across a broad geographic range in Southeast Asia, including Bangladesh, Cambodia, Indonesia, Laos, and Vietnam. By capturing data from multiple countries with varying disease prevalence and healthcare infrastructures, the investigators aimed to create a tool that remains reliable across diverse clinical environments.
The researchers employed a rigorous statistical framework to ensure the reliability of their findings, specifically utilizing external validation (a method where a model is tested on a completely separate dataset to prove it works outside its original training environment). In this process, the data from Cambodia were held out and not used during the initial model training phase. Instead, this independent dataset served as a final test to determine how well the models could predict outcomes in a separate patient population. This step is essential for confirming that the clinical tool is generalizable and not merely calibrated to a single site. For frontline providers, this validation strategy strengthens the evidence that the model can be trusted in real-world primary care settings where rapid, high-stakes referral decisions must be made.
The researchers evaluated a model based on simple clinical parameters to identify children at risk of severe disease, defined as death or the requirement for organ support within two days of presentation. This model achieved a sensitivity of 74.7% (95% CI: 59.4-88.1), indicating a substantial capacity to correctly identify patients requiring urgent intervention. Furthermore, the model demonstrated a high degree of diagnostic accuracy in excluding low-risk cases, reaching a specificity of 99.1% (95% CI: 97.7-99.7). For the practicing clinician, these figures suggest a tool that is highly reliable for confirming which patients can be safely managed in the community, thereby preserving limited hospital resources.
When compared to the established WHO danger signs, the new clinical model showed a marked improvement in diagnostic utility. The WHO criteria showed a sensitivity of 55.5% (95% CI: 39.4-72.7) for identifying children at risk of severe disease, a figure that leaves nearly half of the most critical cases undetected at the initial point of care. Additionally, the WHO criteria showed a specificity of 82.6% (95% CI: 77.1-87.6), which is notably lower than the 99.1% achieved by the new model. This lower specificity in the current WHO standards often leads to a higher volume of unnecessary referrals, placing an avoidable burden on tertiary care facilities.
The clinical implication of these findings is a dual benefit for pediatric triage in resource-constrained settings. By increasing sensitivity from 55.5% to 74.7%, the new model captures a larger proportion of children who are at immediate risk of clinical deterioration. Simultaneously, the increase in specificity to 99.1% ensures that almost all children who are not at risk are correctly identified. This precision minimizes the logistical and financial strain on families and the healthcare system caused by false-positive triage results.
Enhanced Detection via Pulse Oximetry and sTREM1
The diagnostic utility of the clinical models was further enhanced by the integration of objective physiological and biochemical markers. When the researchers incorporated pulse oximetry (a noninvasive method for measuring arterial oxygen saturation) into the assessment, the sensitivity for identifying children at risk of severe disease increased to 88.9% (95% CI: 76.7-97.8). This significant improvement over the basic clinical model suggests that measuring peripheral oxygen levels provides a critical indicator of respiratory or circulatory compromise that may not be immediately apparent through physical examination alone. For the clinician, this means that nearly 90% of children requiring life-saving organ support or at risk of mortality within 48 hours could be identified at the first point of contact using a simple bedside tool.
Beyond physiological monitoring, the study evaluated the addition of soluble triggering receptor expressed on myeloid cells 1, or sTREM1 (a host biomarker that reflects the activation of the innate immune response during infection). Including sTREM1 in the predictive model increased sensitivity to 89.2% (95% CI: 76.9-97.5), a performance level nearly identical to that of pulse oximetry. This biomarker provides a molecular snapshot of the systemic inflammatory response, potentially flagging severe bacterial or viral infections before they manifest as overt clinical instability. While sTREM1 testing requires laboratory capacity, its high sensitivity offers a robust alternative for risk stratification in settings where biochemical screening is feasible.
The clinical efficiency of these enhanced models is particularly evident in their impact on healthcare logistics. The pulse oximetry-based model achieved its sensitivity gains while simultaneously facilitating a threefold reduction in referral rates compared to current standards. By more accurately distinguishing between high-risk patients and those with self-limiting febrile illnesses, this approach ensures that tertiary care resources are reserved for the most critical cases. For practitioners in resource-constrained environments, this reduction in unnecessary referrals alleviates the burden on overstretched hospital systems and reduces the significant financial and emotional strain placed on families during a medical crisis.
Cost-Effectiveness and Future Implementation
Beyond diagnostic accuracy, the economic viability of these triage tools is a critical consideration for health systems in Southeast Asia. The researchers conducted an economic evaluation using the incremental cost effectiveness ratio (ICER), a metric that measures the additional cost required for each additional unit of health benefit gained. The pulse oximetry-based model demonstrated high cost-effectiveness with an ICER of $26.28. In comparison, the model incorporating the host biomarker sTREM1 was also found to be cost-effective, though it yielded a higher ICER of $196.46. These figures suggest that both interventions provide significant clinical value relative to their implementation costs, with pulse oximetry offering a particularly low-cost entry point for improving pediatric outcomes in resource-limited settings.
The researchers concluded that these clinical prediction models could substantially improve triage for acute febrile illness by enabling more accurate referral decisions. By providing a more precise method for identifying children at risk of death or the need for organ support, these tools help clinicians prioritize high-risk patients while avoiding the systemic strain of unnecessary transfers. However, before these models can be integrated into standard practice, the authors noted that they warrant further evaluation in community-based trials. Such prospective studies will be essential to confirm the real-world utility and safety of these algorithms in the hands of frontline health workers across diverse clinical environments.
References
1. Costa F, Hagan JE, Calcagno JI, et al. Global Morbidity and Mortality of Leptospirosis: A Systematic Review. PLoS neglected tropical diseases. 2015. doi:10.1371/journal.pntd.0003898
2. Sangkaew S, Ming D, Boonyasiri A, et al. Risk predictors of progression to severe disease during the febrile phase of dengue: a systematic review and meta-analysis. The Lancet Infectious Diseases. 2021. doi:10.1016/s1473-3099(20)30601-0
3. Evans L, Rhodes A, Alhazzani W, et al. Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock 2021. Critical Care Medicine. 2021. doi:10.1097/ccm.0000000000005337
4. Thompson M, Bruel AVD, Verbakel JY, et al. Systematic review and validation of prediction rules for identifying children with serious infections in emergency departments and urgent-access primary care.. Health Technology Assessment. 2012. doi:10.3310/hta16150
5. Sulis G, Adam P, Nafade V, et al. Antibiotic prescription practices in primary care in low- and middle-income countries: A systematic review and meta-analysis. PLoS Medicine. 2020. doi:10.1371/journal.pmed.1003139
6. Rytter MJH, Kolte L, Briend A, Friis H, Christensen VB. The Immune System in Children with Malnutrition—A Systematic Review. PLoS ONE. 2014. doi:10.1371/journal.pone.0105017