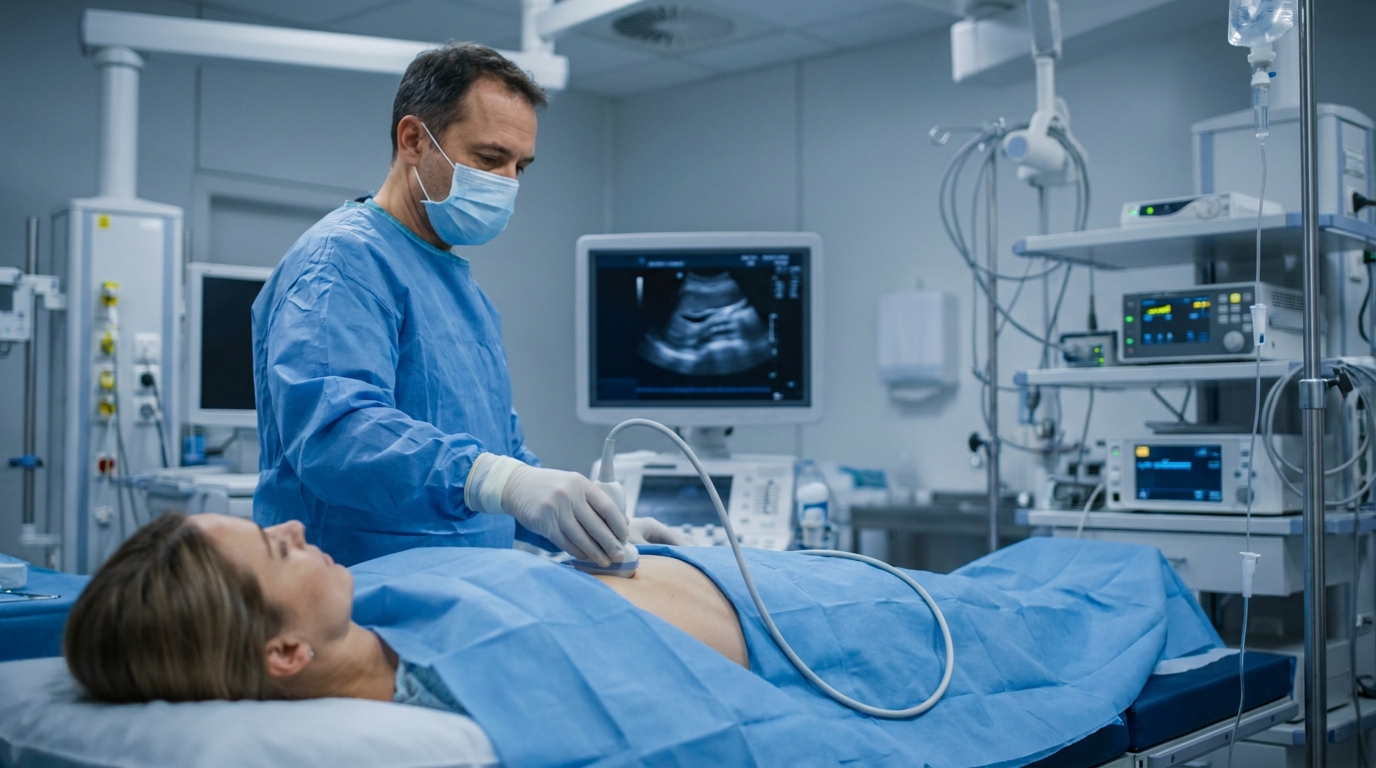
- Umbilical endometriosis causes disabling pain, yet minimally invasive alternatives to surgical excision with proven safety and efficacy remain lacking.
- Researchers evaluated seventeen women with a median age of thirty eight who underwent percutaneous image guided cryoablation for umbilical endometriosis.
- Median pain scores decreased from 8.0 to 0.0 (p < 0.001), with 82 percent of patients achieving complete relief.
- The study concluded that image guided cryoablation is safe and feasible, providing significant nodule reduction and high cosmetic satisfaction.
- This outpatient procedure offers a minimally invasive alternative to surgery for managing umbilical endometriosis while maintaining low patient morbidity.
The Diagnostic and Therapeutic Challenge of Abdominal Wall Endometriosis
Extrapelvic endometriosis remains a complex clinical entity, often presenting as painful nodules within the abdominal wall or surgical scars [1, 2]. While frequently associated with prior obstetric or gynecological procedures, primary cases can occur in the absence of surgical history, which complicates the initial differential diagnosis [3, 4]. Patients typically present with cyclic pain and palpable masses, necessitating high clinical awareness and a multidisciplinary approach to ensure accurate diagnosis [5, 4]. Traditional management has relied heavily on surgical excision, which carries risks of tissue damage and cosmetic dissatisfaction, particularly when lesions are embedded within the rectus abdominis muscle [3, 2]. A recent study evaluates percutaneous image-guided cryoablation, a minimally invasive technique using extreme cold to destroy ectopic tissue under ultrasound or computed tomography guidance, as an alternative to standard surgical approaches [6]. In a cohort of 17 women, this technique achieved complete pain relief in 82% of patients and a 73% median reduction in nodule volume (p < 0.001) at a 22-month median follow-up [6].
Procedural Implementation and Patient Demographics
The study evaluated a cohort of 17 women treated for umbilical endometriosis between March 2017 and December 2024. The median age of the participants was 38 years (interquartile range [IQR], 32 to 38), representing a demographic frequently burdened by symptomatic extrapelvic disease during their peak reproductive years. The researchers utilized percutaneous cryoablation, an interventional radiology technique that involves inserting specialized cryoprobes to deliver extreme cold directly into the lesion. This process induces localized tissue necrosis by freezing the ectopic endometrial glands and stroma while sparing the surrounding healthy abdominal structures. To ensure precise probe placement and monitor the formation of the ice ball, the procedures were performed under ultrasound guidance alone or a combination of ultrasound and computed tomography (CT) guidance. This real-time visualization is critical for umbilical lesions, as it allows clinicians to protect the overlying skin and adjacent bowel from thermal injury. The majority of the interventions were managed without overnight hospitalization, with 16 out of 17 procedures (94%) conducted on an outpatient basis. Although the technique is minimally invasive, the researchers utilized general anesthesia in 12 out of 17 procedures (70%) to ensure patient comfort and prevent any movement during the precise ablation process.
Symptom Resolution and Volumetric Reduction
The clinical efficacy of percutaneous cryoablation was assessed through both subjective pain reporting and objective imaging metrics. At the outset of the study, the researchers established baseline measurements for the umbilical lesions using multiple imaging modalities. The median lesion volume before treatment was 2.42 cm³ (IQR, 0.82 to 4.70) when measured via ultrasound. When evaluated using magnetic resonance imaging (MRI), which provides superior soft tissue contrast for delineating abdominal wall pathologies from surrounding fat and muscle, the median lesion volume was 2.98 cm³ (IQR, 1.14 to 5.49). The primary clinical outcome focused on the alleviation of the cyclic, often debilitating pain characteristic of umbilical endometriosis. Following the procedure, the median peak visual analog scale (VAS) score decreased significantly from 8.0 (IQR, 6.5 to 9.0) at baseline to 0.0 (IQR, 0.0 to 0.0) at follow-up (p < 0.001). This total resolution of symptoms proved durable over time. The study found that complete pain relief was achieved in 14 out of 17 patients (82%) at a median follow-up interval of 22 months (IQR, 12.0 to 31.0). For practicing gynecologists and primary care physicians, this indicates that localized thermal destruction of ectopic tissue can provide long-term symptomatic control without the need for systemic hormonal suppression. In addition to pain management, the researchers documented substantial physical regression of the endometriotic nodules. Post-treatment MRI scans demonstrated that the median nodule volume decreased from 2.98 cm³ to 0.90 cm³. On an individual basis, this represented a median reduction in nodule volume of 73.0% (IQR, 39.3% to 88.4%). This significant volumetric contraction directly addresses the functional discomfort caused by palpable abdominal masses.
Safety Profile and Aesthetic Outcomes
The safety of percutaneous image-guided cryoablation was a primary focus of the study, with complications categorized according to the Society of Interventional Radiology (SIR) classification system. This standardized scale ranks the severity of complications in interventional procedures to guide clinical decision-making. Overall, three adverse events occurred in 17.7% of the study population. Two of these events were classified as minor, specifically SIR Grade B complications involving superficial frostbite. These localized thermal injuries to the skin are a known risk of cryoablation when treating superficial lesions near the dermis, though they typically resolve with conservative management. However, the researchers also documented one major adverse event classified as SIR Grade C, which required subsequent surgical debridement to manage tissue complications at the treatment site. Beyond clinical safety, the study prioritized patient-centered aesthetic results, which are particularly relevant given the highly visible location of umbilical lesions. The researchers found that 82.4% of patients (14 out of 17) reported high levels of cosmetic satisfaction, providing scores of 4 (satisfied) or 5 (very satisfied) on the assessment scale. This high rate of aesthetic success suggests that cryoablation can effectively address the physical deformity caused by umbilical endometriosis without the extensive scarring or umbilicus distortion often associated with traditional surgical excision. For the practicing clinician, these data indicate that percutaneous cryoablation offers a viable, outpatient alternative to surgery. It provides durable symptom relief and preserves abdominal wall aesthetics, broadening the therapeutic options for patients suffering from this rare but debilitating condition.
References
1. Cocco G, Pizzi AD, Scioscia M, et al. Ultrasound Imaging of Abdominal Wall Endometriosis: A Pictorial Review. Diagnostics. 2021. doi:10.3390/diagnostics11040609
2. Tatlı F, GÖZENELİ O, Uyanıkoğlu H, et al. The clinical characteristics and surgical approach of scar endometriosis: A case series of 14 women. Bosnian Journal of Basic Medical Sciences. 2017. doi:10.17305/bjbms.2018.2659
3. Turčić M, Matušan‐Ilijaš K, Molek KR, Zujić PV. Rectus Abdominis Muscle Endometriosis: A Unique Case Report with a Literature Review. Current Issues in Molecular Biology. 2025. doi:10.3390/cimb47010047
4. Cojocari N, Ciutacu L, Lupescu IG, Herlea V, Vasilescu M, Boeți MPS. Parietal Endometriosis: A Challenge for the General Surgeon. Chirurgia. 2018. doi:10.21614/chirurgia.113.5.695
5. Nikolettos K, Patsouras A, Kotanidou S, et al. Pulmonary Endometriosis: A Systematic Review. Journal of Personalized Medicine. 2024. doi:10.3390/jpm14111085
6. Rycke AD, Faure A, Najdawi M, et al. Percutaneous image-guided cryoablation of umbilical endometriosis: safety, feasibility, clinical, and imaging outcomes.. European radiology. 2026. doi:10.1007/s00330-026-12592-7