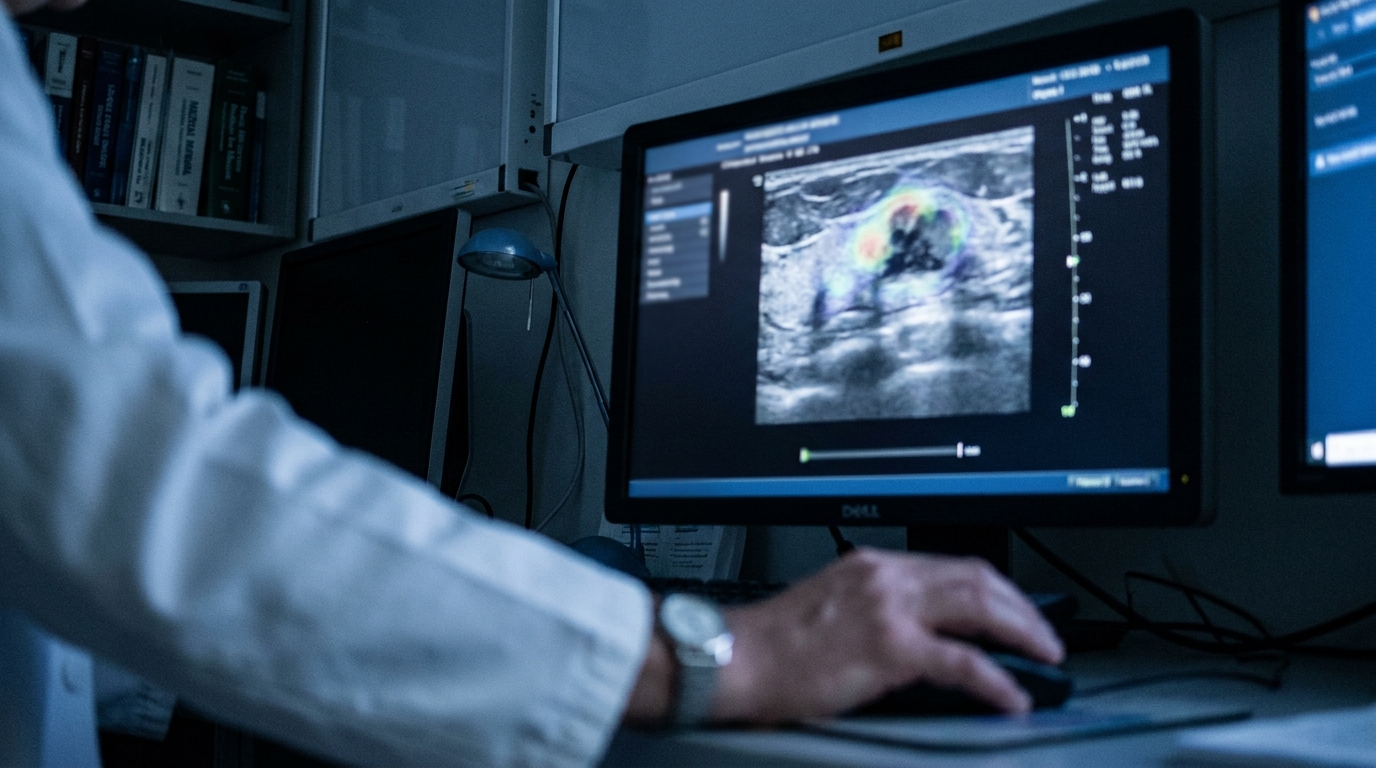
- Clinicians lack a noninvasive method to assess Ki-67 expression, a prognostic marker currently requiring invasive pathological analysis or biopsy.
- Researchers developed a deep learning model using ultrasound and clinical data from 660 patients across four medical centers.
- The model achieved an area under the curve of 0.828 for predicting Ki-67 status in an external test set.
- The findings indicate that high predicted Ki-67 levels correlate with increased lymph metastasis and significantly worse recurrence-free survival.
- This noninvasive tool may assist in preoperative surgical planning and the development of individualized follow-up strategies for breast cancer.
Noninvasive Molecular Profiling in Breast Cancer Imaging
Breast cancer management increasingly relies on precise molecular profiling to guide neoadjuvant and surgical interventions. While ultrasound remains a cornerstone of initial diagnostic imaging, its role has expanded to include the prediction of chemotherapy response and the assessment of axillary lymph node involvement [1, 2, 3]. Meta-analyses indicate that artificial intelligence algorithms integrated into ultrasound workflows can achieve a pooled sensitivity of 0.88 and an area under the curve (AUC) of 0.89 for identifying nodal metastasis [2]. Specifically, the use of deep learning (a subset of artificial intelligence that utilizes multilayered neural networks to identify complex patterns in data) in breast imaging has demonstrated AUCs ranging from 0.868 to 0.909 across various modalities [4, 5]. Recent clinical trial data involving 146 patients further suggest that machine learning models using quantitative ultrasound (a technique that analyzes raw backscattered signals to detect tumor microstructural changes) can predict neoadjuvant treatment response with 92% accuracy and a 99% positive predictive value [6]. These computational techniques offer a noninvasive pathway to identify high-risk features and guide adaptive treatment strategies [7, 6].
Multicenter Model Development and Architecture
To build a noninvasive tool for predicting Ki-67 expression, researchers aggregated data from four distinct medical centers between January 2021 and December 2024. The primary cohort consisted of 456 patients from three centers, partitioned into a training set of 264 patients, a validation set of 96 patients, and an internal test set of 96 patients. To ensure the algorithm could generalize to different clinical environments, the investigators recruited an additional 204 patients from an independent fourth center to serve as an external test set. The dataset incorporated clinical, ultrasound, pathological, and prognostic information to capture a comprehensive view of each patient's disease profile. The core architecture of the deep learning model relied on ResNet-50, a convolutional neural network designed to extract complex, microscopic features from ultrasound images that are typically imperceptible to the human eye. These extracted imaging features were then integrated with standard clinical data through logistic regression, a statistical method used to calculate the probability of a binary outcome, such as high versus low Ki-67 expression. To bridge the gap between algorithmic output and clinical decision-making, the researchers employed class activation mapping, a visualization technique that highlights the specific regions within an ultrasound image that the model prioritized when making its prediction. Furthermore, the study utilized nomograms, which are graphical calculating tools that allow clinicians to estimate the probability of Ki-67 status by combining multiple patient variables. By providing these visual aids, the model offers a transparent process for identifying high-risk pathological features before a patient undergoes an invasive biopsy, streamlining preoperative risk stratification for lymph node metastasis and long-term prognosis.
Predictive Accuracy for Ki-67 and Nodal Status
The current clinical standard for evaluating Ki-67 expression relies on pathological analysis of invasive biopsy samples, a process limited by potential sampling bias and procedural risks. To address these limitations, the researchers validated their deep learning model using the external test set of 204 patients. In this independent cohort, the combined model achieved an area under the curve (AUC) of 0.828 (95% CI: 0.761 to 0.890) for the prediction of Ki-67 status. The AUC is a statistical measure quantifying a model's ability to correctly differentiate between high and low expression levels, where 1.0 represents perfect discrimination. To rigorously assess the model's clinical reliability, the investigators utilized confusion matrices, which are tables that visualize algorithm performance by comparing predicted classifications against actual pathological biopsy results. They also employed calibration curves to determine how closely the predicted probabilities of Ki-67 expression aligned with observed real-world outcomes, alongside decision curve analysis, a method used to estimate the net clinical benefit of using the model across different probability thresholds. Beyond molecular profiling, the model demonstrated significant utility in staging by classifying lymph node metastasis with an accuracy of 0.765. For the practicing oncologist or surgeon, this capability provides a noninvasive method to estimate nodal involvement preoperatively, directly informing the planned extent of surgical intervention and the necessity of axillary lymph node dissection.
Prognostic Stratification and Clinical Utility
The clinical significance of Ki-67 expression lies in its established correlation with breast cancer prognosis and cellular proliferation. To determine the model's utility in a real-world setting, the researchers evaluated its prognostic relevance by examining lymph node metastasis and recurrence-free survival (RFS), defined as the duration of time following primary treatment during which a patient remains free of detectable cancer. The data revealed that the high Ki-67 group experienced significantly higher lymph node metastasis rates compared to the low Ki-67 group (67.7% versus 16.2%, p < 0.001). This stark difference underscores the importance of identifying Ki-67 status early in the diagnostic process to better anticipate the likelihood of axillary disease. Beyond initial staging, the study demonstrated that algorithm-predicted Ki-67 status serves as a critical indicator of long-term outcomes. Patients in the high Ki-67 group showed significantly worse recurrence-free survival than those in the low Ki-67 group (p = 0.041). When assessing the deep learning model's ability to identify patients at risk for early treatment failure, the combined tool achieved an AUC of 0.820 for predicting recurrence in the first 6 months after operation. This high level of predictive accuracy for early recurrence suggests that the model can successfully flag aggressive tumor phenotypes that may require more intensive postoperative surveillance or escalated adjuvant therapy. Ultimately, integrating this deep learning tool into the clinical workflow enables the preoperative prediction of Ki-67 status and lymph metastasis to inform surgical planning. By providing a noninvasive assessment of these high-risk features before the patient enters the operating room, clinicians can better tailor the extent of axillary surgery and refine individualized follow-up strategies, optimizing the timing of systemic interventions based on the predicted biological behavior of the tumor.
References
1. Li Z, Liu X, Gao Y, Lu X, Lei J. Ultrasound-based radiomics for early predicting response to neoadjuvant chemotherapy in patients with breast cancer: a systematic review with meta-analysis.. La Radiologia medica. 2024. doi:10.1007/s11547-024-01783-1
2. Wang M, Liu Z, Ma L. Application of artificial intelligence in ultrasound imaging for predicting lymph node metastasis in breast cancer: A meta-analysis.. Clinical imaging. 2024. doi:10.1016/j.clinimag.2023.110048
3. Li J, Wang S, Li Q, et al. Diagnostic value of multiple ultrasound diagnostic techniques for axillary lymph node metastases in breast cancer: A systematic analysis and network meta-analysis.. Frontiers in oncology. 2022. doi:10.3389/fonc.2022.1043185
4. Aggarwal R, Sounderajah V, Martin G, et al. Diagnostic accuracy of deep learning in medical imaging: a systematic review and meta-analysis. npj Digital Medicine. 2021. doi:10.1038/s41746-021-00438-z
5. Elmejgari C, Nadir Y, Qbadou M. Deep Learning Based Techniques for Breast Cancer Classification: A Systematic Review. 2024. doi:10.1109/IRASET60544.2024.10548784
6. Moore-Palhares D, Alberico D, Chan AW, et al. Quantitative ultrasound imaging for predicting response and guiding personalized neoadjuvant chemotherapy in breast cancer: randomized phase 2 clinical trial results.. NPJ precision oncology. 2025. doi:10.1038/s41698-025-01134-x
7. Liu J, Pian L, Chen J, et al. Artificial intelligence in breast ultrasound: a systematic review of research advances. Frontiers in Oncology. 2025. doi:10.3389/fonc.2025.1619364