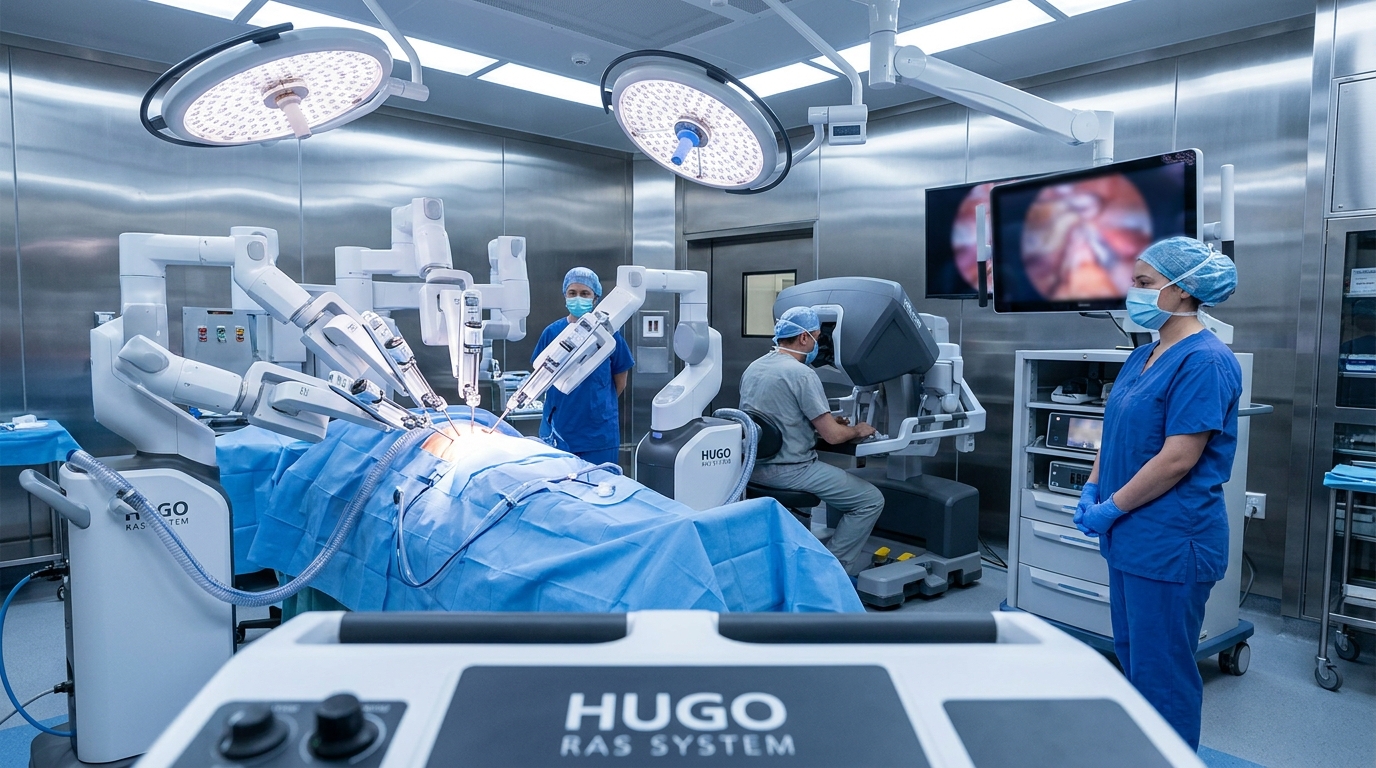
- Researchers evaluated the safety and efficacy of the Hugo robotic-assisted surgery platform for repairing inguinal and ventral hernias in adult patients.
- This prospective, multi-center study enrolled 206 adults, with 193 patients undergoing minimally invasive hernia repair across seven clinical sites.
- The surgical success rate was 100 percent with no conversions, while surgical-site event rates reached 2.1 percent in ventral cases.
- The authors concluded that the Hugo robotic system is safe and effective for performing uncomplicated inguinal and ventral hernia repairs.
- These findings suggest that this robotic platform provides a viable alternative for minimally invasive hernia management in standard clinical practice.
The Evolution of Minimally Invasive Abdominal Wall Reconstruction
Ventral and inguinal hernia repairs remain among the most common procedures in general surgery, with the field increasingly shifting toward minimally invasive techniques to improve patient recovery. While retro-rectus repair (a technique where mesh is placed behind the rectus muscle) is often considered a gold standard for noncomplex ventral hernias, it is associated with higher surgical site infection rates compared to laparoscopic intraperitoneal onlay mesh approaches [1]. Laparoscopic techniques have historically offered faster recovery and fewer complications than open surgery [2], yet robotic-assisted surgery has emerged as a way to potentially combine the benefits of complex myofascial release with lower wound morbidity [3]. Current evidence suggests that while robotic platforms may increase operative time and healthcare costs compared to traditional laparoscopy, they maintain comparable safety profiles and clinical outcomes [4, 5, 6]. As the landscape of surgical technology expands, clinicians require rigorous data to evaluate the performance of specific robotic systems in routine abdominal wall reconstruction.
Trial Design and Patient Selection Criteria
The primary objective of this study was to determine the safety and efficacy of the Hugo robotic-assisted surgery platform for the repair of inguinal and ventral hernias. To evaluate the system within a rigorous clinical framework, the researchers conducted a prospective, multi-center, single-arm trial under an investigational device exemption (a regulatory protocol allowing an unapproved medical device to be used in a clinical study to collect safety and effectiveness data for the Food and Drug Administration). This FDA-approved study was conducted across 7 surgical sites, providing a multi-institutional assessment of the platform's performance in diverse clinical environments. Patient selection focused on establishing a performance baseline by enrolling adults eligible for minimally invasive repair of uncomplicated, non-emergent, and non-recurrent inguinal or ventral hernias. By excluding complex or emergency cases, the study design ensured that the evaluation of the robotic system was not confounded by the technical difficulties inherent in recurrent anatomy or acute surgical pathology. Over an 11-month period, surgeries were performed on a total of 193 patients. For the practicing surgeon, this specific cohort provides a clear measure of the platform's fundamental surgical success and complication rates before considering its application in more high-risk or anatomically challenging abdominal wall reconstructions.
Demographics and Cohort Characteristics
The study initially enrolled 206 adult patients to evaluate the Hugo robotic-assisted surgery platform across multiple clinical sites. Of those enrolled, a total of 193 patients underwent surgical procedures during the 11-month trial period. The researchers divided these participants into two nearly equal groups based on the anatomical location of their pathology, with 97 patients treated in the inguinal hernia cohort and 96 patients treated in the ventral hernia cohort. This distribution ensures that the safety and efficacy data reflect the platform's performance across the two most common types of abdominal wall reconstructions encountered in general surgical practice. The clinical profile of the study population represents a typical demographic for elective hernia repair. The mean age of the participants was 57.4 years (standard deviation 13.6 years), and the mean body-mass index was 28.4 kg/m2 (standard deviation 4.8 kg/m2). A body-mass index in this overweight range is a significant factor for clinicians to consider, as increased truncal adiposity can often complicate the visualization and dissection of the preperitoneal space during minimally invasive approaches. Additionally, the cohort was predominantly male, representing 78.8% (152/193) of the patients, a finding that aligns with the higher physiological incidence of inguinal hernias in men.
Primary Outcomes: Conversion Rates and Surgical Success
The researchers established the primary effectiveness endpoint of the trial as the rate of surgical success. Within the protocol of this multi-center study, surgical success was strictly defined as the procedure not being converted from the use of the Hugo robotic-assisted surgery system to another approach, such as conventional laparoscopy or an open surgical technique. For the practicing clinician, the rate of conversion is a vital indicator of a platform's intraoperative reliability and its ability to facilitate the completion of a planned minimally invasive procedure without the need for unplanned, more invasive maneuvers that can alter the patient's recovery trajectory. The trial data demonstrated a surgical success rate of 100% (193/193), with no conversions to other approaches recorded across the entire study population. This outcome was consistent across both anatomical categories, encompassing all 97 inguinal hernia repairs and all 96 ventral hernia repairs performed during the 11-month period. The absence of any transition to laparoscopic or open methods suggests that the robotic platform provided sufficient visualization and instrument control to manage the technical requirements of these abdominal wall reconstructions in a diverse patient cohort. From a clinical management perspective, the achievement of a 100% success rate in completing the intended robotic approach has direct implications for operating room efficiency and predictable patient outcomes. When a surgical system demonstrates this level of consistency, surgeons can more reliably counsel patients regarding expected incision sizes and postoperative pain levels. Furthermore, the lack of conversions across 193 procedures supports more accurate scheduling and resource allocation within the surgical suite, as unplanned transitions to alternative techniques often result in extended operative times and deviations from standardized recovery protocols.
Safety Profile and 30-Day Postoperative Events
The researchers established the primary safety endpoint as the rate of patients experiencing one or more procedure-related or device-related surgical-site events within a 30-day postoperative window. In the clinical setting, surgical-site events refer to localized complications occurring at the site of the operation, such as surgical site infections, seromas (collections of sterile fluid), hematomas (localized bleeding), or wound dehiscence (the separation of surgical incisions). Monitoring these events through 30 days post-procedure provides a standardized metric for evaluating the immediate safety profile of the robotic platform and its impact on wound healing and early recovery. The clinical data revealed distinct outcomes between the two anatomical cohorts studied. For the 97 patients who underwent inguinal hernia repair, the surgical-site event rate was 0% (0/97), indicating no procedure-related or device-related complications occurred within the first month. In the ventral hernia cohort, which included 96 patients, the surgical-site event rate was 2.1% (2/96). These low rates of localized complications are clinically significant for the practicing surgeon, as they suggest that the robotic system does not introduce additional risk to the integrity of the abdominal wall repair or the healing process compared to established minimally invasive standards. Based on these findings, the study concluded that the Hugo robotic-assisted surgery system is safe and effective for inguinal and ventral hernia repair in a US patient population. For clinicians evaluating new technology, these results provide evidence that the platform maintains a high safety standard across common general surgery procedures. The low incidence of surgical-site events, combined with the previously noted lack of conversions, suggests that the system can be integrated into clinical practice without compromising patient safety or increasing the burden of postoperative wound management.
References
1. Hartog FPJD, Sneiders D, Darwish EF, et al. Favorable Outcomes After Retro-Rectus (Rives-Stoppa) Mesh Repair as Treatment for Noncomplex Ventral Abdominal Wall Hernia, a Systematic Review and Meta-analysis. Annals of Surgery. 2022. doi:10.1097/sla.0000000000005422
2. Lei X, Wang Y, Shan F, et al. Short-and long-term outcomes of laparoscopic versus open gastrectomy in patients with gastric cancer: a systematic review and meta-analysis of randomized controlled trials. World Journal of Surgical Oncology. 2022. doi:10.1186/s12957-022-02818-5
3. Warren JA, Blackhurst DW, Ewing JA, Carbonell AM. Open versus robotic retromuscular ventral hernia repair: outcomes of the ORREO prospective randomized controlled trial. Surgical Endoscopy. 2024. doi:10.1007/s00464-024-11202-1
4. Solaini L, Cavaliere D, Avanzolini A, Rocco G, Ercolani G. Robotic versus laparoscopic inguinal hernia repair: an updated systematic review and meta-analysis. Journal of Robotic Surgery. 2021. doi:10.1007/s11701-021-01312-6
5. Tran E, Sun J, Gundara JS. Systematic review of robotic ventral hernia repair with meta‐analysis. ANZ Journal of Surgery. 2023. doi:10.1111/ans.18822
6. Olavarria OA, Bernardi K, Shah SK, et al. Robotic versus laparoscopic ventral hernia repair: multicenter, blinded randomized controlled trial. BMJ. 2020. doi:10.1136/bmj.m2457