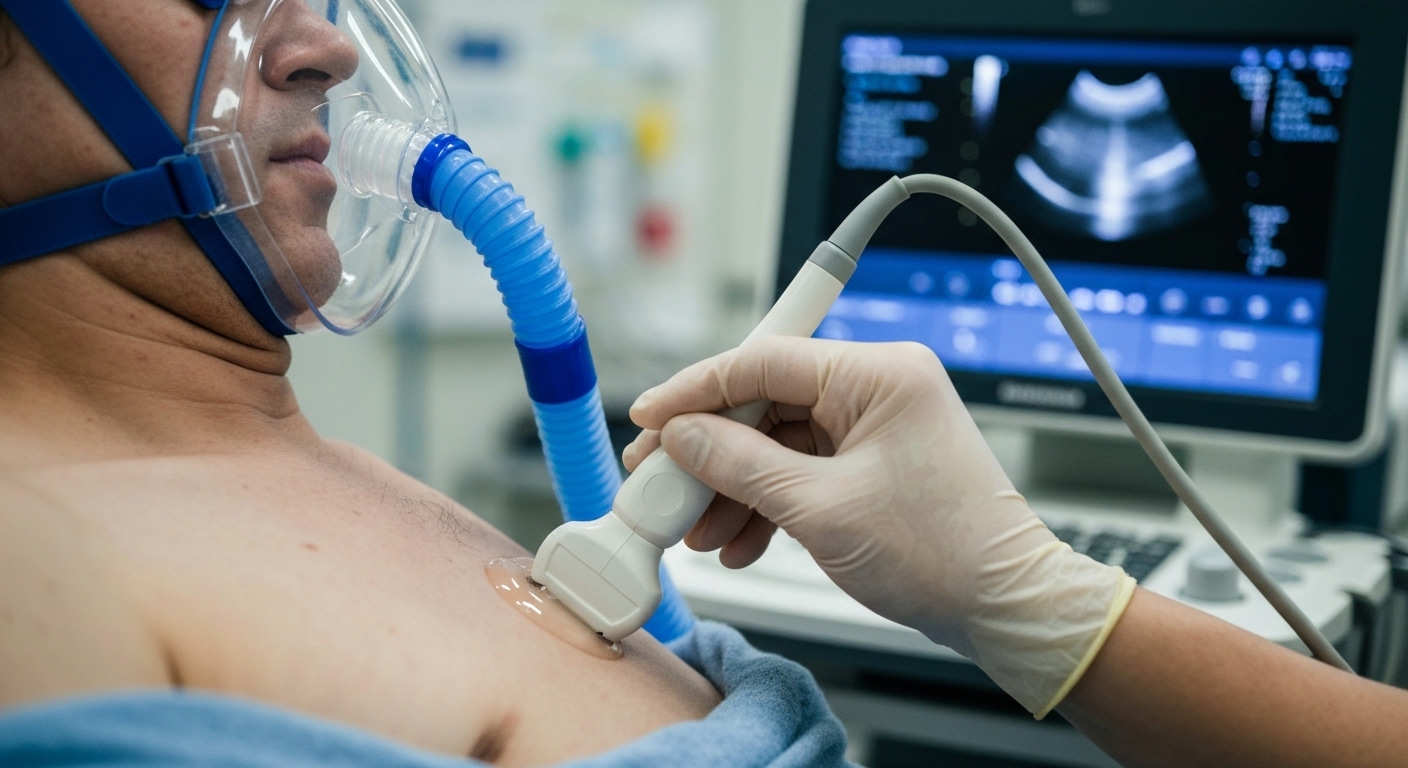
Low Diaphragm Thickening Fraction at One Hour Predicts Noninvasive Ventilation Failure
Bedside ultrasound of the diaphragm after 60 minutes of support identifies patients likely to require endotracheal intubation.
The Clinical Lighthouse
Already a member?
or
The Clinical Lighthouse
Subscribe to read the full analysis
Full access to every article, clinical summary, and the daily evidence brief.
- Unlimited access to all articles
- Daily evidence digest
- Daily podcast with news summaries
- Lighthouse Guideline Briefings
- Ask Lumi: your guide to search, summarise, and explain the archive
- Cancel anytime
