For Doctors in a Hurry
- Surgeons lack clear anatomical definitions of the mandibular septum and its spatial relationship to the marginal mandibular nerve during facelift procedures.
- Researchers performed layer-by-layer dissections on 14 cadavers to map the mandibular septum, adjacent ligaments, and the marginal mandibular nerve.
- The marginal mandibular nerve was located 8.43 to 8.71 millimeters inferior to the mandibular septum at the gonial angle.
- The mandibular septum and platysma-mandibular ligament form a continuous structure that limits jowl fat migration and serves as a surgical landmark.
- Identifying these anatomical relationships helps surgeons avoid nerve injury at the anterior masseter margin where the nerve becomes deeper.
Anatomical Precision in Lower Facial Rejuvenation
Facial rejuvenation surgery remains a cornerstone of aesthetic practice, with techniques ranging from superficial musculoaponeurotic system plication to extended deep-plane dissections [1, 2]. While patient satisfaction rates are generally high, the technical complexity of addressing age-related ptosis and volume loss requires a precise understanding of facial retaining ligaments and fat compartments [3, 4]. Among the most significant surgical risks is iatrogenic injury to the motor nerves, which can result in permanent mimetic deficits and profound psychosocial distress [5, 6]. Revision procedures further complicate these anatomical landmarks due to scarring and altered tissue planes from previous interventions [7]. To mitigate these risks, a recent anatomical study provides a detailed reassessment of the mandibular septum and its critical relationship to the marginal mandibular nerve, offering clinicians precise spatial data to guide safe dissection.
Structural Continuity of the Mandibular Septum
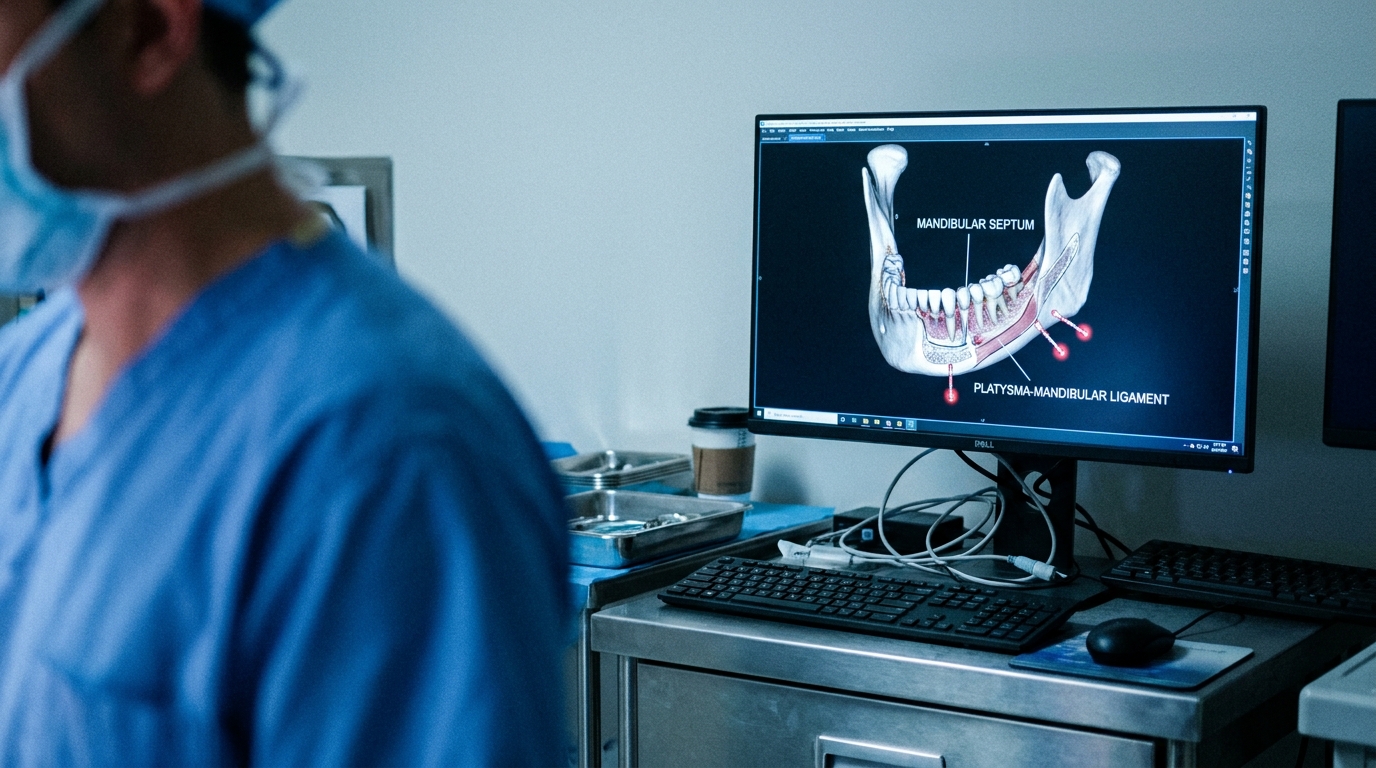
To clarify the structural role and clinical relevance of the mandibular septum, researchers conducted a detailed anatomical investigation using 14 cadavers (28 hemifaces). The mandibular septum is a ligamentous formation that separates the jowl and submandibular fat compartments, acting as a critical boundary in the lower face. To ensure high-resolution visualization of these delicate tissues, the study employed layer-by-layer dissection techniques performed in both the subcutaneous and subplatysmal planes using 3.5x magnifying surgical loupes. This approach allowed for the precise identification of the mandibular septum, the platysma-mandibular ligament (a fibrous attachment between the platysma muscle and the mandible), the mandibular osteocutaneous ligament, and the marginal mandibular nerve. The findings demonstrated that the mandibular septum and the platysma-mandibular ligament are continuous with one another, rather than existing as isolated entities. This continuity creates a unified, supportive structure that limits the inferior migration of jowl fat toward the neck, which is a key factor in the development of an aged lower facial profile. Understanding this anatomy is clinically relevant for surgeons performing facelifts, as it defines the mechanical barriers that must be addressed or preserved to restore a youthful mandibular contour and prevent the descent of soft tissue into the submandibular space.
Spatial Relationships and Surgical Landmarks
To provide a precise vertical map for surgeons navigating the mandibular border, the researchers quantified the spatial relationship between the mandibular septum and the mandibular osteocutaneous ligament (a fibrous band that anchors the skin to the mandible). This ligament serves as a critical landmark during lower face procedures, as its release is often necessary to redrape the skin and improve the jawline contour. The study found that the mandibular osteocutaneous ligament was located 5.79±0.80 mm superior to the platysma-mandibular ligament and mandibular septum on the right side of the face. On the contralateral side, the mandibular osteocutaneous ligament was positioned 5.43±0.94 mm superior to the platysma-mandibular ligament and mandibular septum on the left side. Statistical analysis confirmed that there was no statistically significant difference in the superior distance of the mandibular osteocutaneous ligament between the right and left sides (p>0.05). These measurements establish a consistent anatomical interval of approximately 5.5 to 6.0 millimeters between these two ligamentous structures. For practicing surgeons, this offers a reliable guide for identifying the depth and position of the mandibular septum relative to the more superiorly placed osteocutaneous attachments, facilitating safer and more predictable tissue elevation.
Nerve Preservation and High-Risk Zones
For surgeons performing deep-plane dissections, the marginal mandibular nerve represents a critical structure to avoid, as iatrogenic injury can cause an asymmetric smile and lower lip weakness. The study identified the marginal mandibular nerve at a distance of 8.43±1.91 mm inferior to the mandibular septum at the gonial angle (the posterior corner of the lower jaw) on the right side. On the contralateral side, the marginal mandibular nerve was located 8.71±1.94 mm inferior to the mandibular septum at the gonial angle on the left side. Statistical analysis indicated no statistically significant difference in the inferior distance of the marginal mandibular nerve between the right and left sides (p>0.05). This consistency suggests that the mandibular septum serves as a reliable superior landmark for the nerve's position as it nears the posterior border of the mandible. The researchers observed that the marginal mandibular nerve crossed the mandible exactly at the junction point of the mandibular septum and the platysma-mandibular ligament. After this crossing, the marginal mandibular nerve continued its path preperiosteally (situated just superficial to the periosteum, the dense membrane covering the bone) toward the mental foramen. Throughout its trajectory along the masseter muscle, the marginal mandibular nerve courses inferior to the mandibular septum. However, the depth of the nerve changes significantly as it moves anteriorly. The marginal mandibular nerve becomes deeper at the anterior margin of the masseter muscle, a transition that marks a critical anatomical vulnerability. Consequently, the anterior margin of the masseter is identified as a site where the marginal mandibular nerve is at increased risk of injury during surgical manipulation. Understanding these precise spatial relationships allows clinicians to maintain a safe dissection plane, particularly when releasing the mandibular septum to address jowl descent.
References
1. Meretsky CR, Hausner P, Flynn B, Schiuma AT. A Systematic Review and Comparative Analysis of Reconstructive Rhytidectomy: Advantages, Disadvantages, and Patient Outcomes. Cureus. 2024. doi:10.7759/cureus.71006
2. Mortada H, Alkilani N, Halawani IR, et al. Evolution of Superficial Muscular Aponeurotic System Facelift Techniques: A Comprehensive Systematic Review of Complications and Outcomes. JPRAS Open. 2023. doi:10.1016/j.jpra.2023.06.003
3. Molina-Burbano F, Smith JM, Ingargiola MJ, et al. Fat Grafting to Improve Results of Facelift: Systematic Review of Safety and Effectiveness of Current Treatment Paradigms. Aesthetic Surgery Journal. 2020. doi:10.1093/asj/sjaa002
4. Williams EF, Urban MJ. Trials, Tribulations, and Techniques for Transitioning to an Extended Deep Plane Facelift for All Patients: Insight from a Very Experienced Surgeon's Perspective. Facial Plastic Surgery. 2024. doi:10.1055/s-0044-1779626
5. Gandra G, Silva BMD, Horta R. Facelift Surgery and Nerve Injury: A Systematic Review and Meta-Analysis. Aesthetic Plastic Surgery. 2025. doi:10.1007/s00266-025-04932-7
6. Guntinas‐Lichius O, Prengel J, Cohen O, et al. Pathogenesis, diagnosis and therapy of facial synkinesis: A systematic review and clinical practice recommendations by the international head and neck scientific group. Frontiers in Neurology. 2022. doi:10.3389/fneur.2022.1019554
7. ŞİBAR S, Erdal AI, Genç G. Revision Neck Lift Surgery: A Systematic Review of Indications, Techniques, and Outcomes. Aesthetic Plastic Surgery. 2026. doi:10.1007/s00266-026-05686-6