For Doctors in a Hurry
- Clinicians lack standardized non-invasive methods for measuring intracranial pressure despite the risks associated with current gold-standard invasive monitoring techniques.
- This review evaluates multiple non-invasive modalities including optic nerve sheath diameter and transcranial Doppler blood flow velocity across various clinical settings.
- Transcranial Doppler methods show 95 percent limits of agreement of plus or minus 7 to 15 mmHg compared to invasive monitoring.
- The researchers conclude that combining different modalities and advanced signal analysis may improve the predictive accuracy of these indirect measurements.
- These techniques help clinicians identify intracranial hypertension early in the emergency department to prevent missing the critical golden hour of care.
Expanding the Reach of Neurocritical Monitoring
Managing intracranial hypertension remains a cornerstone of neurocritical care, particularly in traumatic brain injury where monitoring-guided strategies are linked to improved prognosis [1]. While invasive monitors are the established gold standard, their use is often restricted by clinical contraindications such as coagulopathy or the lack of specialized neurosurgical resources [2]. Furthermore, cerebral hypoxia can occur even in the absence of overt intracranial hypertension, complicating the management of patients with severe brain injury [3]. In the broader intensive care setting, conditions like sepsis and acute liver failure also necessitate vigilant neurological assessment to prevent secondary damage [4, 5]. A recent review evaluates how non-invasive techniques may bridge these diagnostic gaps across diverse clinical environments, offering clinicians alternative tools when direct catheterization is not feasible.
Clinicians currently have access to several non-invasive techniques that serve as surrogates for invasive intracranial pressure monitoring when traditional catheters are contraindicated. Among the most established is transcranial Doppler blood flow velocity assessment, which evaluates cerebral hemodynamics via arterial or venous vessels. This method provides a physiological snapshot of cerebral perfusion, though its precision is constrained by challenges in calibration and zeroing. Specifically, the researchers noted that for transcranial Doppler-based methods, the 95% limits of agreement are approximately ± 7 to 15 mmHg compared to invasive gold standards. Another vascular-based approach is double-depth ophthalmic artery blood flow velocity measurement, a technique that compares flow in the intraorbital and intracranial segments of the ophthalmic artery to estimate pressure.
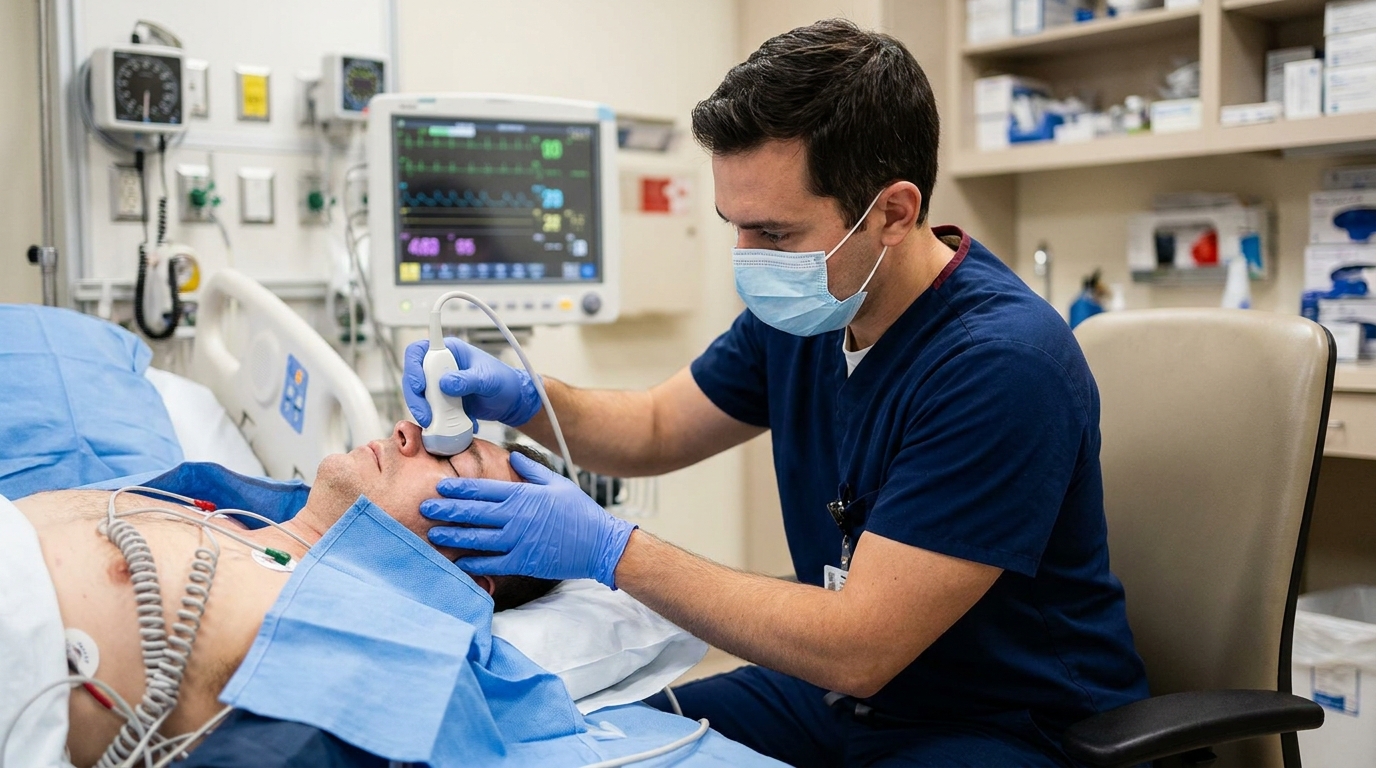
For structural assessments, clinicians can measure the optic nerve sheath diameter using ultrasound to evaluate the nerve envelope, which expands as cerebrospinal fluid pressure rises. This technique demonstrates slightly tighter precision than Doppler methods, with 95% limits of agreement ranging from ± 7 to 10 mmHg. Automated pupillometry, which uses infrared sensors to provide a quantitative measurement of the pupillary light reflex, offers another non-invasive surrogate for intracranial pressure assessment. Beyond bedside ultrasound and pupillometry, standard brain imaging helps identify structural markers of elevated pressure, such as midline shift or ventricular effacement. More specialized techniques include the measurement of skull expansion and compliance (a method that detects minute changes in cranial volume in response to pressure fluctuations) and ultrasound time-of-flight (a technique that measures the speed of sound across the cranium to estimate pressure changes). While these individual modalities face accuracy constraints, the authors suggest that combining different tools and applying advanced signal analysis may improve predictive accuracy, ultimately helping physicians make safer triage decisions in diverse patient populations.
Quantifying the Accuracy Gap
While invasive methods remain the gold standard for intracranial pressure measurement due to their direct nature, non-invasive monitoring remains insufficiently recognized in clinical practice. This limited adoption is primarily driven by the technical challenges of achieving parity with direct catheterization. The researchers identified that calibration and zeroing (the process of establishing a reliable baseline and reference point) are the main limitations of all indirect methods. These hurdles constrain the absolute accuracy of non-invasive monitoring, as clinicians cannot always ensure that the surrogate values reflect the true physiological state without a physical zero point.
The study quantified the precision of these tools using the 95% limits of agreement, a statistical measure representing the range within which 95% of the differences between the non-invasive and invasive measurements are expected to fall. For transcranial Doppler-based methods, the 95% limits of agreement are approximately ± 7 to 15 mmHg. Techniques based on the optic nerve sheath diameter demonstrate slightly narrower 95% limits of agreement ranging from ± 7 to 10 mmHg. These margins suggest that while these tools are highly useful for trend monitoring, their absolute values may deviate significantly from gold-standard measurements, requiring physicians to interpret the data alongside the broader clinical picture.
To address these discrepancies, the authors suggest that predictive accuracy may be improved by combining different modalities, such as integrating vascular flow data with anatomical measurements. Furthermore, applying advanced signal analysis techniques (the use of computational processing to interpret complex physiological waveforms) may help refine these estimates. By synthesizing data from multiple sensors and using sophisticated algorithms to filter out noise, clinicians may be able to narrow the current accuracy gap and better manage patients when invasive monitoring is contraindicated.
Clinical Applications from the Emergency Department to the ICU
In the emergency department, early detection of intracranial hypertension helps prevent missing the golden hour of brain care, the critical initial window where rapid intervention is required to mitigate secondary neurological injury. For patients presenting with acute brain injury, non-invasive methods can guide patient selection for urgent invasive monitoring. This allows clinicians to prioritize high-risk individuals for direct catheterization while potentially avoiding the procedure in lower-risk cases. These techniques also facilitate brain assessment in moderate traumatic brain injury, a clinical category where patients may not initially meet the criteria for invasive sensors but still require close neurological surveillance to detect delayed swelling or hematoma expansion.
The utility of these tools extends to the general intensive care population, where non-invasive monitoring assists management in patients with coagulopathy (a condition characterized by impaired blood clotting). In such cases, the risk of intracranial hemorrhage during the placement of an invasive pressure transducer often outweighs the benefits, making indirect assessment a necessary alternative. Furthermore, these methods provide valuable information after cardiac arrest, liver failure, and sepsis, systemic conditions that can lead to cerebral edema and elevated pressures through metabolic or inflammatory pathways. Finally, non-invasive intracranial pressure monitoring is particularly relevant in low-resource settings where specialized neurosurgical expertise and intensive care facilities are limited. By leveraging these accessible tools, physicians can maintain a high standard of neurocritical care even in environments where gold-standard invasive technology is unavailable.
References
1. Uparela-Reyes MJ, Ordoñez-Cure S, Moreno-Drada J, Villegas-Trujillo LM, Escobar-Vidarte OA. Diagnostic Accuracy of Optic Nerve Sheath Diameter Measurement by Ultrasonography for Noninvasive Estimation of Intracranial Hypertension in Traumatic Brain Injury: A Systematic Review and Meta-Analysis.. Neurosurgery. 2024. doi:10.1227/neu.0000000000003273
2. Connolly ES, Rabinstein AA, Carhuapoma JR, et al. Guidelines for the Management of Aneurysmal Subarachnoid Hemorrhage. Stroke. 2012. doi:10.1161/str.0b013e3182587839
3. Pustilnik HN, Medrado-Nunes GS, Cerqueira GA, et al. Brain tissue oxygen plus intracranial pressure monitoring versus isolated intracranial pressure monitoring in patients with traumatic brain injury: an updated meta-analysis of randomized controlled trials.. Acta neurochirurgica. 2024. doi:10.1007/s00701-024-06125-8
4. Dellinger RP, Levy MM, Carlet J, et al. Surviving Sepsis Campaign: International guidelines for management of severe sepsis and septic shock: 2008. Intensive Care Medicine. 2007. doi:10.1007/s00134-007-0934-2
5. Rhodes A, Evans L, Alhazzani W, et al. Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock: 2016. Critical Care Medicine. 2017. doi:10.1097/ccm.0000000000002255