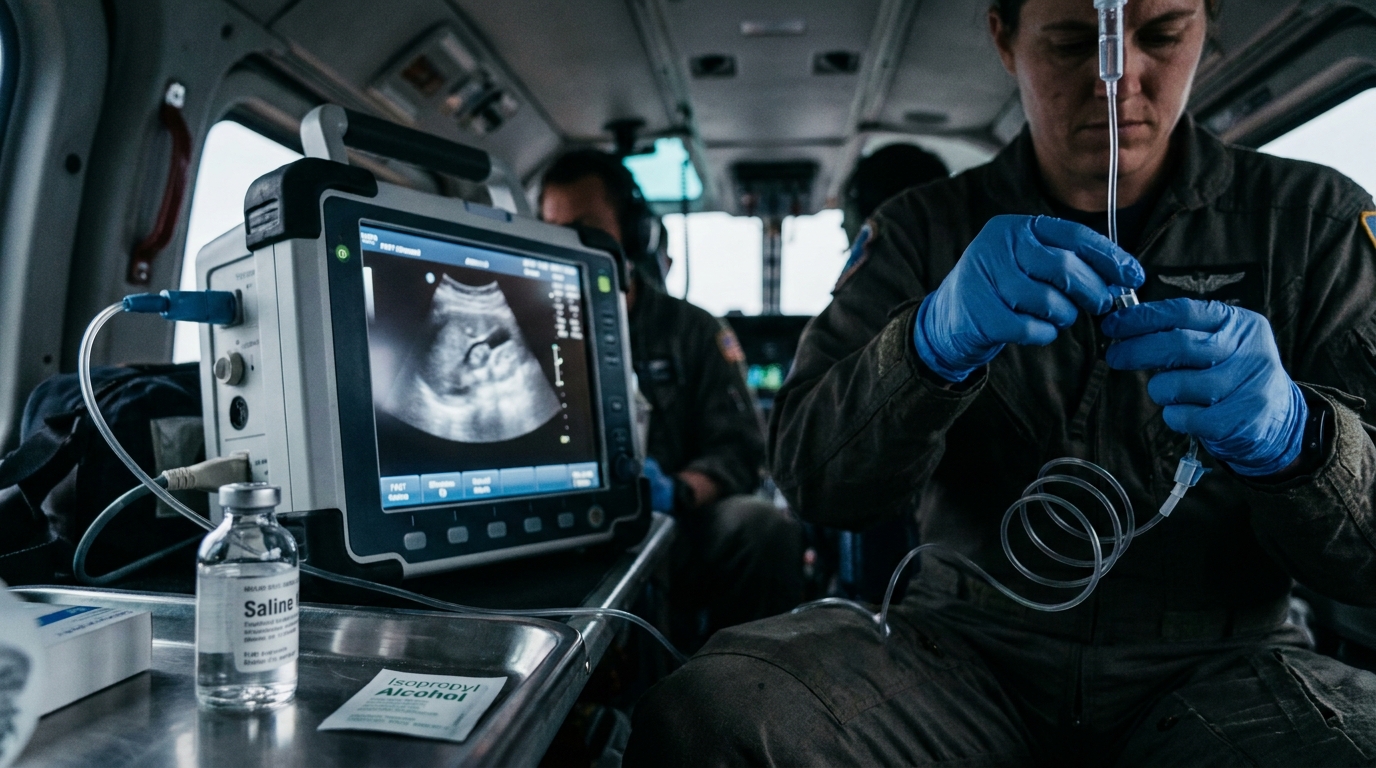
- Researchers investigated whether prophylactic ondansetron or isopropanol aromatherapy reduces opioid-induced nausea during prehospital emergency care for traumatic pain.
- This prospective study analyzed 205 patients receiving opioids, comparing 4 mg intravenous ondansetron, isopropanol inhalation, or no prophylaxis.
- All groups showed a median change of 0 on the Numeric Rating Scale, with nausea increasing in 14 to 15 percent of patients.
- The researchers concluded that neither ondansetron nor aromatherapy provides a significant benefit for preventing nausea in unselected prehospital patients.
- Clinicians should reconsider routine prophylaxis in this setting until larger trials identify specific subgroups that might benefit from these interventions.
Reevaluating Antiemetic Prophylaxis in Acute Pain Management
Opioid-induced nausea and vomiting remain significant challenges in acute care, often complicating pain management and potentially delaying patient discharge [1]. While 5-hydroxytryptamine receptor 3 (serotonin) antagonists like ondansetron are established standards for preventing postoperative symptoms [2, 3, 4], their efficacy varies significantly across different clinical triggers and patient populations [5]. Non-pharmacological interventions, including aromatherapy and acupuncture, are frequently explored as adjuncts to reduce the side effect burden of traditional analgesics [6, 7]. However, the utility of routine prophylaxis in the high-acuity prehospital environment is less clear, as interventions that succeed in controlled surgical settings may not translate to the emergency transport of trauma patients. A new prospective study evaluates whether these common prophylactic strategies actually provide clinical benefit during helicopter emergency medical evacuations [8].
A Quasi-Experimental Comparison of Three Prophylactic Strategies
The researchers conducted a prospective study between February 2024 and April 2025 involving crews from six helicopter emergency medical services bases. The study population consisted of patients over the age of 16 who required opioid therapy for acute traumatic pain. To evaluate the efficacy of different interventions, the authors utilized a quasi-experimental design (a methodology that lacks random assignment but uses structured protocols to compare groups) based on a fixed rotating 7-day schedule. This structure assigned patients to one of three distinct study arms: no nausea prophylaxis, medication-based prophylaxis with ondansetron 4 mg intravenously, or aromatherapy-based prophylaxis via the inhalation of isopropanol. Clinical assessment of nausea relied on a numeric rating scale, where 0 represented no nausea and 10 represented the maximum possible nausea. Clinicians recorded these scores at two specific time points: the moment of opioid administration and upon patient handover at the destination hospital emergency department. The primary endpoint was defined as the change in numeric rating scale score between these two points. Additionally, the researchers tracked several secondary endpoints to capture the clinical burden of symptoms, including the incidence of moderate and severe nausea (defined as a score greater than 3), the occurrence of vomiting during prehospital care, and the requirement for rescue medication in the form of therapeutic ondansetron administration.
Minimal Impact on Nausea Scores and Vomiting Incidence
The final analysis included a total of 205 patients who received prehospital opioid therapy for traumatic pain. This cohort was distributed across three study arms, with 86 patients in the no prophylaxis group, 64 patients in the ondansetron group, and 55 patients in the aromatherapy group. Across all three cohorts, the researchers found a median change in numeric rating scale scores of 0 points, with an interquartile range of 0 to 0. This indicates that for the majority of patients, the intensity of nausea remained unchanged from the time of opioid administration to hospital handover, regardless of whether they received a prophylactic intervention. When examining individual patient trajectories, the incidence of worsening symptoms was nearly identical between the groups. An increase in nausea scores occurred in 15% of patients in the no prophylaxis group, 14% of patients in the ondansetron group, and 15% of patients in the aromatherapy group. Furthermore, the frequency of clinically significant symptoms, defined as a score greater than 3, was observed in 14% of patients who received no prophylaxis and in 11% of patients in both the ondansetron and aromatherapy arms. These findings suggest that routine prophylactic administration does not substantially alter the subjective experience of nausea in the acute prehospital setting. The incidence of emesis remained low across the entire study population. Vomiting occurred in 4% of patients in the no prophylaxis group and 2% of patients in the ondansetron group, while 0% of patients in the aromatherapy group experienced emesis. Although the aromatherapy group reported no vomiting, the overall low frequency of this event across all arms limits the clinical impact of the intervention. For practicing physicians, this suggests that the baseline risk of severe opioid-induced nausea during short transport times may be too low to justify universal preventative treatment.
Clinical Implications for Prehospital Emergency Protocols
The study also evaluated the efficacy of reactive interventions when prophylactic measures were either absent or ineffective. Therapeutic rescue administration of ondansetron was necessary in 4 patients in the no prophylaxis group and in 1 patient in the aromatherapy group. These rescue efforts yielded poor clinical results in the acute prehospital window. Specifically, none of the patients who received rescue medication experienced any improvement in nausea as a result of the administration. The lack of efficacy for rescue therapy was further highlighted by the fact that three patients from the no prophylaxis group vomited after receiving rescue ondansetron administration. This suggests that once opioid-induced symptoms begin in the trauma setting, standard antiemetic doses may fail to provide rapid stabilization before hospital arrival. Based on the lack of significant difference in nausea scores and the failure of rescue interventions, the researchers concluded that neither prophylactic ondansetron nor aromatherapy appear beneficial for preventing opioid-induced nausea in unselected prehospital emergency patients. For the practicing clinician, these findings indicate that the routine, reflexive administration of antiemetics alongside opioid analgesics in the field may not be a necessary component of standard trauma protocols. While the data show no clear benefit for the general trauma population, the authors noted that larger randomized controlled trials are required to determine if specific high-risk subgroups might still benefit from these interventions. In the interim, these results support a more selective approach to antiemetic therapy during emergency transport, allowing clinicians to avoid unnecessary medication administration without compromising patient comfort.
References
1. Yadeau J, Fields K, Kahn R, et al. Readiness for Discharge After Foot and Ankle Surgery Using Peripheral Nerve Blocks: A Randomized Controlled Trial Comparing Spinal and General Anesthesia as Supplements to Nerve Blocks. Anesthesia and Analgesia. 2018. doi:10.1213/ANE.0000000000003456
2. Worravitudomsuk T, Charuluxananan S, Sukumpanumet W, Sriprajittichai P. A Randomized, Controlled Trial of Palonosetron Versus Ondansetron for Nausea, Vomiting, and Pruritus in Cesarean Delivery with Intrathecal Morphine. Anesthesia and Analgesia. 2024. doi:10.1213/ANE.0000000000007091
3. Worravitudomsuk T, Charuluxananan S, Sukumpanumet W, Sriprajittichai P. REGIONAL ANESTHESIA A Randomized, Controlled Trial of Palonosetron Versus Ondansetron for Nausea, Vomiting, and Pruritus in Cesarean Delivery With Intrathecal Morphine. Obstetric Anesthesia Digest. 2025. doi:10.1097/01.aoa.0001125588.23942.3e
4. Hajian P, Malekianzadeh B, Davoudi M. Efficacy of Intravenous Ondansetron on Hemodynamic Complications in Women Undergoing Spinal Anesthesia for Cesarean Section: A Randomized Placebo Controlled Clinical Trial. Galen medical journal. 2016. doi:10.31661/gmj.v5i1.475
5. Kazemi-Kjellberg F, Henzi I, Tramèr MR. Treatment of established postoperative nausea and vomiting: a quantitative systematic review. BMC Anesthesiology. 2001. doi:10.1186/1471-2253-1-2
6. Greenlee H, DuPont‐Reyes MJ, Balneaves LG, et al. Clinical practice guidelines on the evidence‐based use of integrative therapies during and after breast cancer treatment. CA A Cancer Journal for Clinicians. 2017. doi:10.3322/caac.21397
7. Cheong KB, Zhang J, Huang Y, Zhang Z. The Effectiveness of Acupuncture in Prevention and Treatment of Postoperative Nausea and Vomiting - A Systematic Review and Meta-Analysis. PLoS ONE. 2013. doi:10.1371/journal.pone.0082474
8. Knapp J, Strohm R, Huber M, Albrecht R, Pietsch U. Prophylaxis of opioid-induced nausea in helicopter emergency medical service: a prospective quasi-experimental study. Scandinavian Journal of Trauma Resuscitation and Emergency Medicine. 2026. doi:10.1186/s13049-026-01626-0