- This study investigated if sutureless off-clamp robotic partial nephrectomy is noninferior to renorrhaphy for surgical quality.
- A single-center randomized controlled trial assigned 248 patients with cT1-2N0M0 renal tumors to either technique.
- Trifecta achievement, the primary endpoint, was 93% for sutureless and 95% for renorrhaphy, with a 90% CI of -7.4% to 2.6%.
- The authors concluded that sutureless off-clamp robotic partial nephrectomy is safe, effective, and a feasible alternative.
- This technique offers clinicians an additional surgical option for selected cT1-2N0M0 renal tumor patients.
Advancing Nephron-Sparing Surgery for Renal Tumors
Nephron-sparing surgery, particularly robotic partial nephrectomy (RPN), is the established standard for managing clinical T1 renal masses, a shift driven by the rising incidental detection of small tumors and the clinical imperative to preserve long-term renal function [1, 2]. The central challenge of RPN is to achieve complete tumor excision while minimizing iatrogenic damage to healthy kidney tissue, a balance demanding highly refined surgical techniques [3]. The success of these procedures is often measured by composite outcomes like the "Trifecta," a metric combining negative surgical margins, minimal warm ischemia time, and the absence of major complications [4, 5]. As robotic platforms evolve, so do the surgical approaches, with a continuous effort to improve patient safety and functional outcomes [6, 7]. For instance, recent analyses show that while novel robotic systems yield similar surgical and clinical outcomes to established platforms [6], specific techniques like tumor enucleation may be associated with fewer complications and better kidney function compared to standard resection, all while maintaining oncologic control [7]. This landscape of incremental refinement sets the stage for evaluating new modifications to RPN.
Evaluating a Sutureless Approach for Renal Tumor Resection
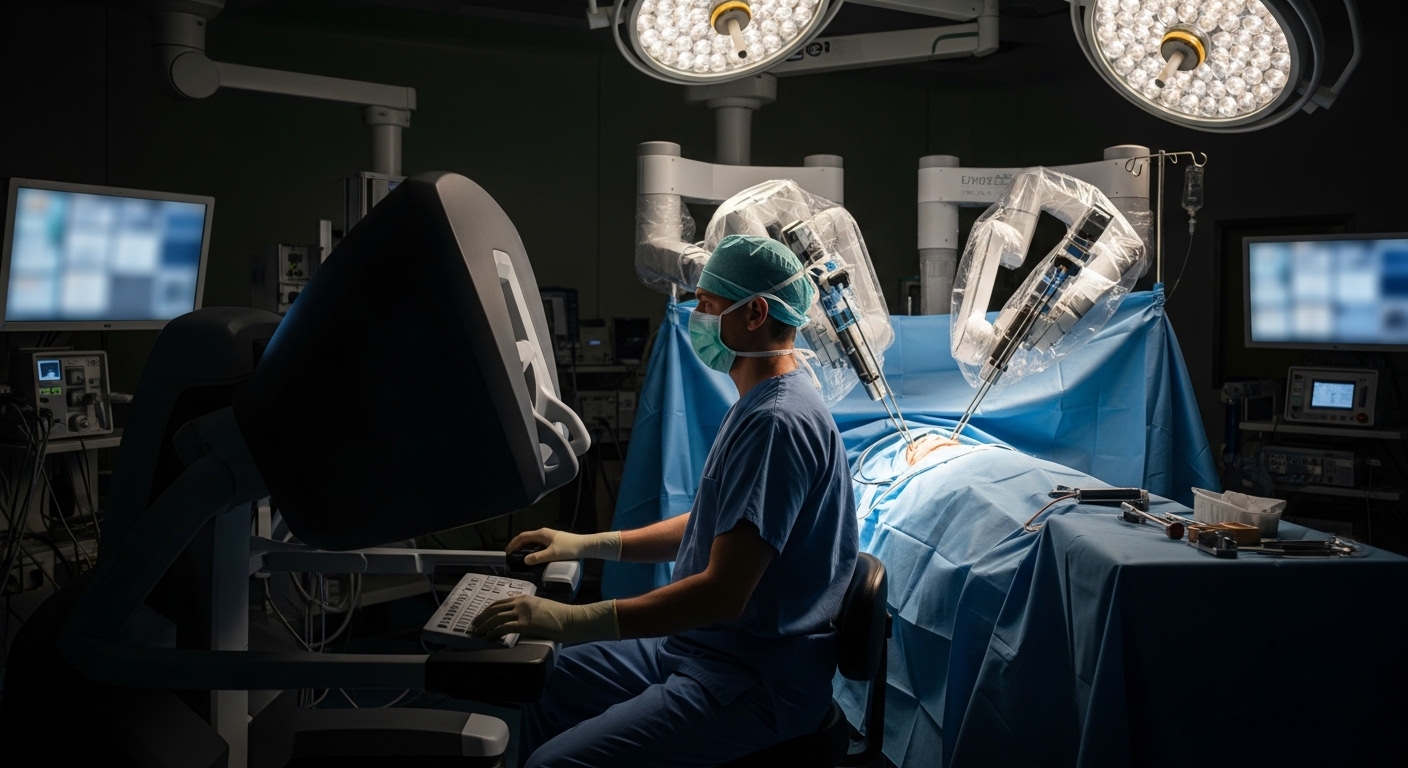
To further minimize postoperative renal damage, a sutureless, purely off-clamp robotic partial nephrectomy (SL-ocRPN) technique has been developed. This approach avoids both vascular clamping and the subsequent suturing of the renal parenchyma, known as renorrhaphy (RR), thereby aiming to reduce ischemic injury and parenchymal trauma. To rigorously test this method, a new study directly compared its surgical quality against the conventional renorrhaphy technique. The investigation was designed as a single-center, single-surgeon randomized controlled trial (NCT06846112) involving patients with cT1-2N0M0 renal tumors. Participants were assigned in a 1:1 ratio to either SL-ocRPN or RR-ocRPN. To ensure a fair comparison, the researchers used a covariate-adaptive randomization algorithm, a statistical method that actively balances prognostic factors like age, sex, baseline renal function, and tumor complexity between the two treatment groups, minimizing the risk of selection bias.
Defining Surgical Success and Statistical Rigor
The study's primary measure of success was the achievement of the Trifecta at discharge. This composite endpoint provides a holistic assessment of surgical quality by requiring the simultaneous fulfillment of three criteria: negative surgical margins for complete cancer removal, an acceptable warm ischemia time to limit kidney damage, and the absence of major postoperative complications. To determine if the sutureless technique was a valid alternative to the established standard, the researchers designed a noninferiority trial. This type of trial aims to show that a new treatment is not unacceptably worse than the current one. A prespecified noninferiority margin was set at -10%, meaning the sutureless approach would be considered noninferior if its Trifecta success rate was no more than 10 percentage points lower than that of the renorrhaphy group. This hypothesis was tested using one-sided statistical tests and confidence intervals. Secondary outcomes were also analyzed to provide a broader picture of safety and efficacy, while long-term oncologic control was assessed by estimating recurrence-free survival (RFS) using the Kaplan-Meier method, a standard statistical technique for analyzing survival data over time.
Noninferiority Confirmed for Primary Endpoint
The trial included 248 patients, with baseline characteristics well-balanced between the sutureless (SL) and renorrhaphy (RR) arms, confirming the success of the randomization strategy. The primary endpoint analysis revealed high rates of surgical quality in both groups. Trifecta was achieved in 93% of patients undergoing the sutureless procedure compared to 95% of those in the renorrhaphy group. This resulted in an absolute difference of -2.4%, with a 90% confidence interval (CI) ranging from -7.4% to 2.6%. Because the lower bound of this confidence interval (-7.4%) did not cross the prespecified noninferiority boundary of -10%, the sutureless technique met the formal criterion for noninferiority. This was further supported by a one-sided p-value of 0.006, providing strong statistical evidence that SL-ocRPN is not clinically inferior to RR-ocRPN for achieving excellent surgical quality in patients with cT1-2N0M0 renal tumors.
Comparable Safety and Functional Outcomes
An analysis of secondary outcomes further supported the clinical utility of the sutureless technique. Major adverse events were infrequent in both cohorts. The need for blood transfusions was low, occurring in 2.4% of the sutureless group versus 0% of the renorrhaphy group. The incidence of acute kidney injury was identical and rare, at 1.6% in both arms. A total of nine urinary fistulae occurred across the study, and while the rate was numerically higher in the sutureless group, the difference did not reach statistical significance (p = 0.08). Critically, all fistulae were managed successfully with temporary stenting, avoiding the need for more invasive reintervention. From a functional and oncologic standpoint, the outcomes were excellent and equivalent. Renal function remained stable in all patients up to 12 months post-surgery, and the one-year recurrence-free survival was 99% across all cohorts. These findings demonstrate that the sutureless approach maintains patient safety and achieves robust short-term cancer control.
Clinical Implications and Study Considerations
This randomized trial provides strong evidence that sutureless off-clamp robotic partial nephrectomy is a safe and effective procedure for selected renal tumors. The findings confirm that it is a feasible alternative to conventional renorrhaphy for cT1-2N0M0 tumors, delivering noninferior surgical quality. For practicing urologic surgeons, this means SL-ocRPN can be considered a valid technical option, potentially simplifying the operative procedure by eliminating parenchymal suturing without compromising immediate surgical success, patient safety, or short-term oncologic outcomes. However, clinicians should interpret these findings within the context of the study's limitations. The single-center design and the use of a single, highly experienced surgeon mean that these excellent results may not be immediately generalizable to all practice settings or surgeons with less robotic experience. Furthermore, the short oncologic follow-up of one year necessitates longer-term data to confirm durable cancer control and renal function preservation. Despite these caveats, the study offers valuable, high-quality evidence supporting SL-ocRPN as a sound surgical choice for appropriate patients in centers with established expertise in robotic surgery.
References
1. Bamias A, Escudier B, Sternberg CN, et al. Current Clinical Practice Guidelines for the Treatment of Renal Cell Carcinoma: A Systematic Review and Critical Evaluation. The Oncologist. 2017. doi:10.1634/theoncologist.2016-0435
2. Guerrero ER, Claro AVO, Cepero MJL, Delgado MS, Fernández JLÁ. Robotic versus Laparoscopic Partial Nephrectomy in the New Era: Systematic Review.. Cancers. 2023. doi:10.3390/cancers15061793
3. Pandolfo SD, Wu Z, Campi R, et al. Outcomes and Techniques of Robotic-Assisted Partial Nephrectomy (RAPN) for Renal Hilar Masses: A Comprehensive Systematic Review. Cancers. 2024. doi:10.3390/cancers16040693
4. Bai N, Mu-ge Q, Shan D, Liu S, Ta N, Chen L. Trifecta achievement in patients undergoing partial nephrectomy: a systematic review and meta-analysis of predictive factors. International braz j urol. 2022. doi:10.1590/s1677-5538.ibju.2021.0095
5. Artsitas S, Artsitas D, Segkou I, Tsourouflis G, Dimitroulis D, Nikiteas N. Considering “Trifecta” as a Single Outcome when Comparing Robotic With Open Partial Nephrectomy: A Mathematical Model of Volume Conservation and Systematic Review. In Vivo. 2022. doi:10.21873/invivo.12992
6. Rossi F, Sighinolfi MC, Gavi F, et al. Novel multiport robotic systems versus da vinci multiport robotic system in robot-assisted partial nephrectomy: a systematic review and meta-analysis of surgical and oncological outcomes. Journal of Robotic Surgery. 2026. doi:10.1007/s11701-026-03277-w
7. Bertolo R, Pecoraro A, Carbonara U, et al. Resection Techniques During Robotic Partial Nephrectomy: A Systematic Review. European Urology Open Science. 2023. doi:10.1016/j.euros.2023.03.008