For Doctors in a Hurry
- Clinicians require accurate, noninvasive alternatives to chest radiography for diagnosing pneumonia in pediatric patients to reduce radiation exposure.
- This review analyzed multiple meta-analyses comparing the diagnostic performance of point-of-care lung ultrasound against traditional clinical assessments and radiography.
- Lung ultrasound demonstrated a sensitivity of 94 percent and a specificity of 96 percent for identifying pediatric pneumonia.
- The researchers concluded that ultrasound provides high diagnostic accuracy while offering bedside applicability and eliminating ionizing radiation risks.
- Physicians should integrate standardized ultrasound protocols and clinical correlation to differentiate bacterial pneumonia from viral infections or asthma.
Advancing Bedside Diagnostics for Pediatric Respiratory Infection
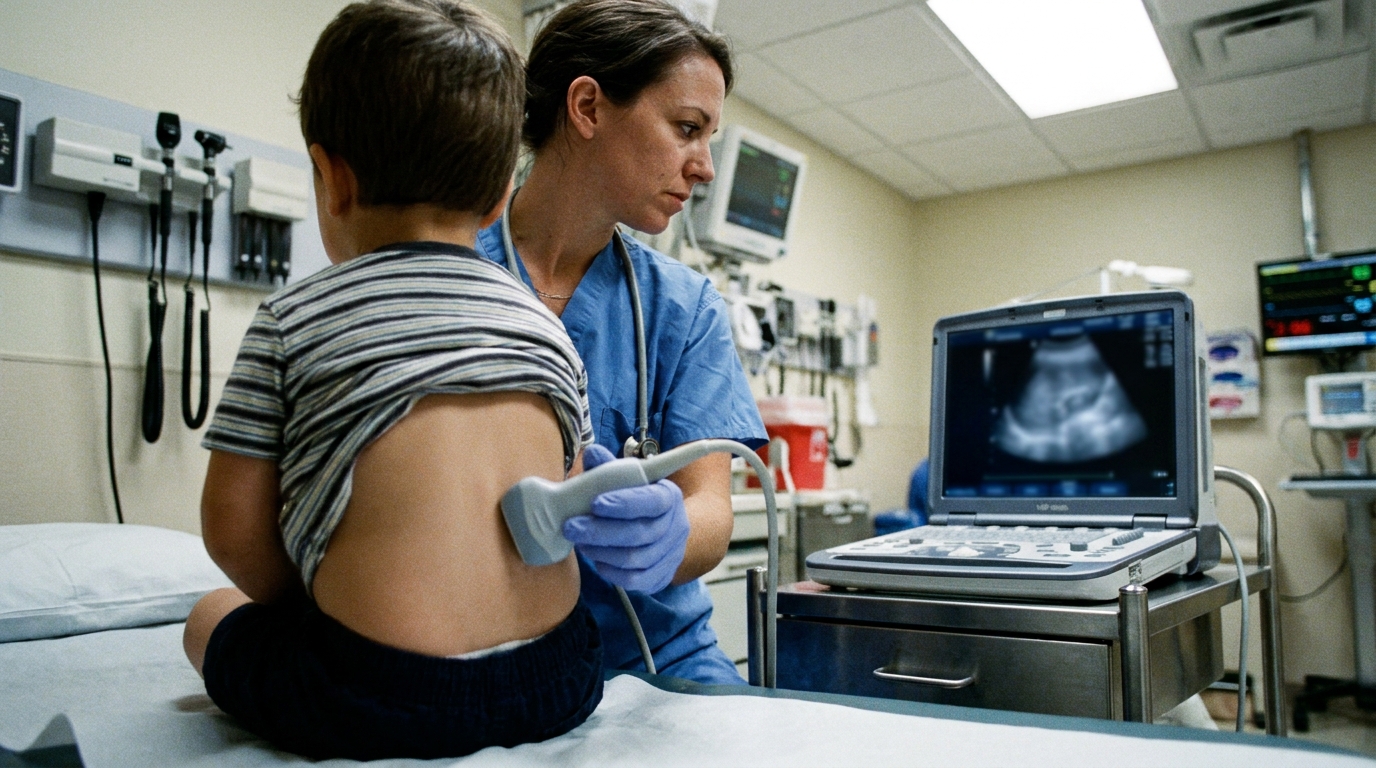
Pneumonia remains a primary driver of pediatric morbidity and mortality, necessitating rapid diagnostic strategies in acute care environments [1, 2]. While chest radiography is the traditional standard, the risks of ionizing radiation and logistical delays of fixed imaging present significant clinical hurdles [3, 4]. Consequently, clinicians are increasingly adopting point-of-care lung ultrasound (a bedside imaging technique that identifies pleural irregularities and subpleural consolidations) to expedite diagnosis [5]. Recent meta-analytic data encompassing 4,546 children show that lung ultrasound yields a pooled sensitivity of 94.0% (95% CI: 93.0% to 94.9%) and a specificity of 85.5% (95% CI: 83.5% to 87.3%) for community-acquired pneumonia [4]. Although the modality is operator-dependent, advanced sonographers maintain a high area under the receiver operating characteristic curve (a statistical measure of overall diagnostic accuracy) of 0.97 [5]. The current review further examines the clinical integration of these ultrasound protocols in pediatric populations, evaluating how physicians can safely incorporate them into daily practice.
Comparative Accuracy and Resource Efficiency
Physicians traditionally rely on clinical examination and chest radiography to evaluate suspected pediatric pneumonia. However, point-of-care lung ultrasound has emerged as a noninvasive alternative for diagnosing this condition in children. The current review evaluates the diagnostic accuracy, benefits, and limitations of lung ultrasound in direct comparison with clinical assessment and chest radiography. By analyzing these modalities, the researchers aimed to determine if sonography can reliably supplement or replace standard imaging in acute pediatric settings. Data from multiple meta-analyses indicate that lung ultrasound provides high diagnostic precision. Specifically, the modality offers a sensitivity of up to 94% and a specificity of up to 96% for the diagnosis of pediatric pneumonia. These metrics demonstrate that the diagnostic performance of lung ultrasound is comparable to, and in some instances exceeds, the performance of chest radiography. This high level of accuracy is particularly relevant for clinicians who must rapidly differentiate pneumonia from other respiratory distress etiologies in a fast-paced emergency department or clinic. Beyond diagnostic metrics, lung ultrasound offers several practical advantages for the practicing physician. A primary benefit is the elimination of ionizing radiation exposure, which is a critical component of pediatric stewardship. Furthermore, the technique allows for immediate bedside applicability, enabling the physician to perform the scan and interpret results concurrently with the physical examination. This streamlined workflow is associated with lower costs compared to traditional imaging modalities, making it a resource-efficient tool for both inpatient and outpatient pediatric care.
Diagnostic Overlap and Interpretation Challenges
Despite the high diagnostic accuracy reported in recent meta-analyses, the researchers emphasize that significant challenges remain in standardizing the interpretation of lung ultrasound findings. Unlike traditional radiography, which benefits from decades of established reporting conventions, point-of-care sonography is highly operator-dependent. The study notes that the lack of universally accepted protocols and diagnostic algorithms can lead to variability in how different clinicians interpret pulmonary artifacts and consolidations. This lack of standardization necessitates rigorous clinician training to ensure the modality is used effectively within routine pediatric respiratory care. A primary clinical limitation identified by the authors is that distinguishing bacterial pneumonia from viral illness or asthma is difficult due to overlapping ultrasound findings. These distinct etiologies can present with similar sonographic markers, such as subpleural consolidations or B-lines (vertical artifacts that indicate interstitial fluid or inflammation). Because a consolidated lung segment or a focal area of B-lines can appear in multiple disease states, the imaging findings alone are often insufficient to isolate a specific causative agent. Because of these diagnostic ambiguities, the researchers conclude that overlapping ultrasound findings in pediatric respiratory conditions require careful clinical correlation to avoid misdiagnosis and inappropriate antibiotic use. The physician must integrate sonographic data with the patient history, physical examination, and laboratory markers to differentiate between infectious pneumonia and other forms of respiratory distress. While lung ultrasound provides a high level of sensitivity, its role is most effective when used as a supplement to comprehensive clinical judgment.
Requirements for Clinical Integration
To maximize the clinical utility of lung ultrasound in pediatric care, the researchers emphasize that standardized protocols are essential. These protocols provide a consistent framework for image acquisition and interpretation, reducing the variability inherent in operator-dependent diagnostics. Furthermore, clinician training is required to ensure that practitioners can accurately identify sonographic markers of pneumonia and distinguish them from normal anatomy or benign artifacts. Beyond technical proficiency, the study notes that diagnostic algorithms are necessary to guide clinical decision-making, helping physicians systematically integrate ultrasound findings with other clinical data to reach a definitive diagnosis. While the current data supports the high diagnostic accuracy of this modality, the authors conclude that further research is warranted to refine the differentiation between bacterial and viral etiologies using ultrasound. Currently, overlapping sonographic features can complicate the distinction between these causes of respiratory distress, which has direct implications for targeted antibiotic stewardship. Additionally, the researchers state that further research is needed to effectively integrate lung ultrasound into routine clinical pathways, ensuring that the transition from traditional radiography to point-of-care sonography is seamless, evidence-based, and practical for busy pediatric care settings.
References
1. Orso D, Ban A, Guglielmo N. Lung ultrasound in diagnosing pneumonia in childhood: a systematic review and meta-analysis.. Journal of ultrasound. 2018. doi:10.1007/s40477-018-0306-5
2. Guitart C, Becerra J, Bobillo-Perez S, et al. Diagnostic Accuracy of Lung Ultrasound for Pneumonia in Acutely and Critically Ill Neonates, Children, and Young Adults: A Systematic Review and Meta-Analysis.. Diagnostics (Basel, Switzerland). 2025. doi:10.3390/diagnostics15243122
3. Abid I, Qureshi N, Lategan N, Williams S, Shahid S. Point-of-care lung ultrasound in detecting pneumonia: A systematic review.. Canadian journal of respiratory therapy : CJRT = Revue canadienne de la therapie respiratoire : RCTR. 2024. doi:10.29390/001c.92182
4. Shi C, Xu X, Xu Y. Systematic review and meta-analysis of the accuracy of lung ultrasound and chest radiography in diagnosing community acquired pneumonia in children.. Pediatric pulmonology. 2024. doi:10.1002/ppul.27221
5. Tsou P, Chen KP, Wang Y, et al. Diagnostic Accuracy of Lung Ultrasound Performed by Novice Versus Advanced Sonographers for Pneumonia in Children: A Systematic Review and Meta-analysis.. Academic emergency medicine : official journal of the Society for Academic Emergency Medicine. 2019. doi:10.1111/acem.13818